- What Are Managed IT Services for Healthcare?
- Why Managed IT Services Are Vital in Healthcare — With Real Use Cases
- Benefits of Managed IT Services in Healthcare
- The Real Cost Comparison: In-House IT vs. Managed IT Services
- How Managed IT Services for Healthcare Improve Patient Outcomes
- Managed IT Services vs. Break-Fix Model: Full Comparison
- What a Managed IT Services Implementation Actually Looks Like
- 5 Common Mistakes Healthcare Organizations Make With IT
- Components of Managed IT Services for Healthcare
- Managed IT Services vs. Break-Fix Model
- How to Choose a Managed IT Service Provider
- 5 Key Takeaways for Healthcare Leaders Evaluating Managed IT Services
- Conclusion
- Ready to Build a Secure, HIPAA-Compliant IT Foundation?
Unlike other sectors, healthcare directly impacts lives. This necessitates rigorous vetting and careful implementation of any new technology. Technology plays a pivotal role in enhancing patient care, streamlining operations, and ensuring compliance with stringent regulations.
A misconfigured firewall rule doesn’t just mean lost productivity — it can expose protected health information (PHI), trigger six-figure HIPAA fines, or delay access to patient records during a critical care moment. Yet most hospitals, clinics, and digital health companies are not resourced to manage enterprise-grade security, compliance, and infrastructure in-house around the clock.
That’s the exact gap Managed IT Services for Healthcare exist to close. In this updated guide — built from real implementation experience and SEO-audited for relevance — you’ll find detailed use cases, honest cost breakdowns, a step-by-step migration timeline, the most common healthcare IT mistakes, and a structured checklist for selecting the right MSP. Everything a CTO, COO, or IT Director at a healthcare organization needs to make a confident, well-informed decision.
What Are Managed IT Services for Healthcare?
A Managed Service Provider (MSP) in healthcare takes ongoing, contractual responsibility for your IT environment under a fixed service agreement. Unlike a staffing model (where you pay for time) or break-fix (where you pay per incident), an MSP is accountable for outcomes — defined uptime percentages, security response times, compliance posture, and audit readiness.
The typical scope of Managed IT Services for Healthcare includes:
- Infrastructure monitoring & management — servers, networking, endpoints, virtual machines, cloud resources — with 24/7 alerting
- Cybersecurity operations — SIEM, Endpoint Detection & Response (EDR), vulnerability scanning, patch management, penetration testing
- HIPAA compliance management — technical safeguards, administrative documentation, audit trail maintenance, and annual risk assessment
- EHR and clinical application support — Epic, Cerner, Allscripts integrations, HL7 FHIR interoperability, uptime monitoring for clinical systems
- Cloud services with HIPAA BAA — AWS, Azure, or GCP environments with Business Associate Agreements, encryption at rest and in transit
- Backup and Disaster Recovery (DRaaS) — automated daily backups, immutable storage, tested recovery with defined RPO/RTO SLAs
- 24/7 service desk — tiered support for clinical staff, administrative teams, and IT escalations
- Vendor and license management — single point of accountability for all your technology relationships
Managed IT services refer to outsourcing IT management and support to a specialized provider, known as an MSP. These providers handle a wide array of responsibilities, such as:
- Network and infrastructure management
- Cybersecurity and threat detection
- Software updates and patching
- Data backups and compliance tracking
For healthcare, MSPs specifically ensure uptime, secure handling of patient data, and seamless operation of critical systems like EHRs and diagnostic tools.
Why Managed IT Services Are Vital in Healthcare — With Real Use Cases
1. HIPAA Compliance Is an Ongoing Architecture Problem, Not a One-Time Checklist
HIPAA’s Security Rule requires continuous technical safeguards, documented administrative controls, and physical security measures — all of which must be audit-ready at any moment, not just in the weeks before a scheduled review. Most organizations treat HIPAA as an annual exercise. Enforcement actions tell a different story: the HHS Office for Civil Rights imposed over $135 million in penalties across documented enforcement actions, with the majority stemming from failures in ongoing security management, not one-time events.
An MSP embeds compliance into the infrastructure itself rather than layering it on afterward:
- Role-based access controls on all PHI-touching systems, reviewed quarterly
- Immutable audit logs for every PHI access event — who, when, from where
- Automatic account deprovisioning when staff exit
- Continuous monitoring mapped to HIPAA Security Rule controls
- Documented risk assessments updated when systems or threats change
“The most dangerous assumption in healthcare IT is that HIPAA compliance is a one-time checkbox. Regulations evolve, systems change, and threat actors adapt. Compliance monitoring must be continuous — not annual.”— Roman Burdiuzha, Co-founder & CTO, Gart Solutions
Real use case: A regional hospital group ran a legacy on-premise EHR platform with no encryption at rest and shared administrative credentials across IT staff. An HHS inquiry triggered an internal audit that revealed nine separate Security Rule deficiencies. Gart Solutions managed a 14-week cloud migration to a HIPAA-compliant AWS environment: encryption enabled, MFA enforced, audit logging active, and all nine deficiencies remediated with documentation. The alternative — uncontested HHS fines — would have been between $100 and $50,000 per violation category per year. See how Gart’s Compliance Audit Services work in practice.
2. Healthcare Is the #1 Target for Cyberattacks — and the Least Prepared
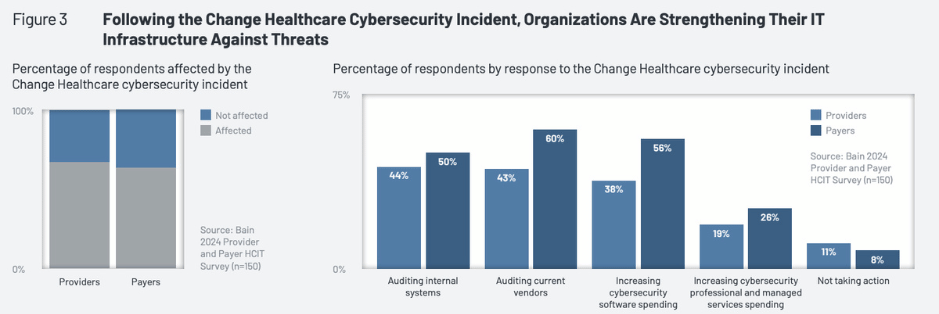
Healthcare records are worth significantly more on dark web markets than financial records, because they contain a uniquely complete package: identity, insurance data, prescription history, Social Security numbers, and medical conditions that can be exploited for insurance fraud, identity theft, and targeted scams. The HHS reports a 93% increase in large healthcare data breaches between 2018 and 2022, with ransomware now accounting for the majority of incidents.
A mature managed security posture for healthcare includes:
- 24/7 SIEM monitoring with healthcare-specific threat intelligence feeds
- EDR on all clinical workstations, laptops, and BYOD devices with EHR access
- Privileged Access Management (PAM) for EHR admin accounts and infrastructure
- Ransomware-resilient backups: immutable storage, air-gapped copies, tested recovery
- Regular phishing simulations and staff security awareness training
- Network segmentation to isolate medical devices from administrative systems
Real use case: A digital health startup running a remote patient monitoring platform had no formal security monitoring in place — just a basic firewall and antivirus. After a near-miss phishing incident that almost compromised a clinician’s EHR credentials, they engaged a managed security partner. Within 30 days, the MSP deployed a SIEM with HIPAA-mapped alert rules, configured EDR on all endpoints, and during the initial environment scan identified three misconfigured cloud storage buckets that were exposing patient monitoring data. All three were remediated before a breach occurred. Learn more about Gart’s IT Monitoring Services and how continuous monitoring works in regulated healthcare environments.
3. Complex Clinical System Ecosystems Require Specialized Expertise
Most healthcare facilities run 8–15 interconnected clinical and administrative systems: EHR platforms, PACS imaging systems, lab information systems (LIS), patient portals, telehealth platforms, scheduling software, and billing applications. Each integration point is a potential failure point, a potential security gap, and a potential compliance risk.
A healthcare-specialized MSP maintains:
- HL7 FHIR and HL7 v2 expertise for interoperability between clinical systems
- API-level monitoring between systems — catching latency and data sync failures before clinicians experience them
- Change management processes for clinical software updates that schedule maintenance windows around care workflows, not just technical convenience
- Validated testing environments that mirror production without exposing real PHI
Benefits of Managed IT Services in Healthcare
Proactive Security
Threats detected and neutralized before they impact care delivery or trigger compliance violations.
Continuous HIPAA Compliance
Automated evidence collection, audit-ready documentation, and regulatory change monitoring built-in.
Predictable Costs
Fixed monthly fees replace unpredictable break-fix invoices and eliminate emergency staffing premiums.
Elastic Scalability
Infrastructure scales from a single clinic to a multi-site network — without procurement delays.
99.9%+ Uptime SLA
Contractual availability guarantees for EHR, scheduling, and diagnostic systems.
Clinical-First Focus
IT burden removed from clinical leadership so medical teams can prioritize patient outcomes.
1. Proactive Maintenance
Continuous network monitoring and scheduled updates prevent issues before they impact staff or patients.
- Continuous monitoring prevents issues before they disrupt operations.
- Regular software updates ensure compatibility and security.
Fixed monthly fees reduce budget surprises. Leasing hardware and tailored service plans optimize costs.
High IT costs can strain budgets. Gart Solutions helps mitigate this by offering leasing options and tailored services that reduce hardware expenditures while maintaining high-quality IT support.
- Simplifies budgeting by avoiding unexpected expenses.
- Ensures critical systems are always operational, saving revenue and protecting patient care.
3. Scalability
Services expand or contract as practices grow, from solo clinics to multi-location facilities.
As healthcare practices expand, their IT needs evolve. MSPs can scale services as practices grow, from single practitioners to multi-location facilities.
Gart Solutions provides flexible and scalable solutions to support growth, ensuring technology keeps pace with increasing demands without compromising efficiency.
4. Focus on Core Activities
By outsourcing IT management, healthcare providers can concentrate on patient care rather than troubleshooting technical issues.
5. Enhanced Patient Care
Reliable IT systems reduce wait times, improve diagnostic workflow, and enable better provider–patient communication.
6. Cybersecurity & Compliance
Healthcare is a prime target for cyberattacks. MSPs deliver encryption, 24/7 monitoring, disaster recovery, and ensure HIPAA, GDPR, and HITECH compliance.
The Real Cost Comparison: In-House IT vs. Managed IT Services
The most common objection to MSP engagement is cost. The honest answer requires calculating total cost of ownership — not just the MSP contract price — against the fully-loaded cost of in-house IT. When healthcare organizations do this analysis properly, the results are usually decisive.
| Cost Factor | In-House IT Team (3 FTE) | Managed IT Services (MSP) |
|---|---|---|
| Staff salaries + benefits | $240,000–$360,000 / yr | Included in monthly contract |
| Security tools & licenses | $30,000–$80,000 / yr | Included (shared cost model) |
| Staff training & certifications | $15,000–$25,000 / yr | Included |
| 24/7 coverage | Requires additional shift hire or on-call premium | Standard in MSP agreements |
| HIPAA compliance expertise | Separate consultant: $150–$300/hr | Included |
| Disaster recovery testing | Rarely budgeted; rarely executed | Scheduled, documented, SLA-backed |
| Recruitment & turnover cost | $20,000–$60,000 per hire replaced | Zero — MSP absorbs attrition |
| Typical total annual cost | $380,000–$620,000+ | $80,000–$220,000 (mid-size org) |
MSP pricing varies by scope, size, and complexity. Request a scoped proposal for your specific environment — a credible MSP will provide itemized cost breakdowns with no hidden variables.
How Managed IT Services for Healthcare Improve Patient Outcomes
The link between IT reliability and patient outcomes is direct, measurable, and still under-discussed when healthcare leaders evaluate MSP options. Here’s the practical connection:
- Reduced wait times: When scheduling and EHR systems are reliably available, front-desk staff process check-ins faster and clinicians access records without “EHR is slow today” delays becoming a chronic part of care delivery
- Faster diagnostic workflows: PACS and LIS uptime directly determines radiology and lab turnaround times. A 30-minute PACS outage during a busy morning shifts delays downstream into the entire care workflow for hours
- Telehealth reliability: With remote consultations now a permanent feature of healthcare delivery, cloud infrastructure quality and video platform uptime have become direct patient safety variables — not just IT metrics
- Reduced medication errors: Integrated, always-available clinical systems reduce workarounds. Workarounds (paper, verbal orders, memory) are where medication errors are born
- Ransomware recovery capability: In a ransomware attack, an MSP with tested DRaaS can restore clinical systems in hours — not the weeks that self-managed recovery often requires. The difference is measured in diverted ambulances, cancelled procedures, and patient transfers
For documented examples of how infrastructure quality affects clinical operations, see Gart’s work on digital transformation in healthcare.
Managed IT Services vs. Break-Fix Model: Full Comparison
| Aspect | Break-Fix Model | Managed IT Services |
|---|---|---|
| Core approach | Reactive: respond after failure occurs | Proactive: prevent failure before it happens |
| Cost model | Unpredictable; spikes during incidents | Fixed monthly fee; budget certainty |
| HIPAA compliance | Out of scope by default | Built in; continuously monitored |
| Security monitoring | None between incidents | 24/7 SIEM + EDR + threat response |
| Downtime | High; only addressed after impact | Minimal; issues surfaced by monitoring |
| Disaster recovery | Rarely planned; discovered during crisis | Designed, tested, SLA-documented |
| Vendor management | Ad hoc; customer’s responsibility | MSP-owned; coordinated proactively |
| Contractual accountability | Time & materials; no outcome SLA | SLAs with financial consequences |
| Best fit | Very small, low-risk, non-regulated | Any regulated healthcare environment |
What a Managed IT Services Implementation Actually Looks Like
The most common concern healthcare leaders express before engaging an MSP is disruption: “What happens to our EHR access during the transition? What if clinical staff can’t log in?” A well-designed onboarding is built around that concern from day one — zero clinical downtime is a hard requirement, not an aspiration.
Here is a realistic implementation timeline for a mid-size healthcare organization (100–500 staff, 2–5 locations):
Discovery & Infrastructure Audit
Full inventory of all hardware, software, clinical systems, user accounts, and cloud resources. Security posture baseline established. HIPAA gap analysis completed. Zero changes to production systems.
Monitoring & Visibility Deployment
Monitoring agents deployed across all managed systems. SIEM configured with HIPAA-mapped alert rules. SLA clock begins. Dashboard and reporting configured for client visibility. Clinical workflows untouched.
Security Hardening
Critical vulnerabilities remediated. MFA enforced on all EHR and admin accounts. Stale user accounts audited and deprovisioned. Patch management cadence established. HIPAA technical safeguard documentation updated.
Backup & Disaster Recovery
Automated backup policies configured with HIPAA-compliant storage. First full recovery test executed and documented (RPO/RTO validated against contract SLAs). Incident response runbooks written and tested with the clinical operations team.
Cloud Migration (IF APPLICABLE)
Workloads migrated to HIPAA-compliant cloud environment using a parallel-run strategy. Old and new environments run simultaneously until validation is complete. Zero-downtime cutover executed during lowest-activity window.
Steady-State Operations + Continuous Improvement
Monthly security reports. Quarterly compliance posture reviews. Annual HIPAA risk assessment. Continuous monitoring, patching, and user support. Roadmap reviews tied to your clinical and operational growth plans.
5 Common Mistakes Healthcare Organizations Make With IT
Based on infrastructure audit findings across dozens of healthcare environments, these are the patterns that appear most consistently — regardless of organization size or budget. Understanding them helps avoid the expensive remediation they typically require.
Treating security as an afterthought
Building clinical systems for functionality first and “adding security later” creates architectural debt that is expensive to fix and frequently incomplete. HIPAA-compliant security must be designed in from the first infrastructure decision — encryption policies, access controls, and audit logging cannot be reliably retrofitted.
Assuming cloud = compliant
AWS, Azure, and GCP offer HIPAA-eligible infrastructure, but compliance is a shared responsibility model. The cloud provider secures the physical layer; everything built on top — configurations, access controls, audit logging — is the customer’s responsibility. A signed BAA is necessary but not sufficient.
Never actually testing backup restoration
Backup success metrics only show data was copied. They do not confirm a full restoration is possible. Most organizations discover their backups don’t work during a ransomware incident. HIPAA requires a tested contingency plan with documented results.
Accumulated over-privileged accounts
Without automated deprovisioning, organizations accumulate former employees with active EHR access and staff with admin-level permissions they don’t need. This is among the most common HIPAA audit findings and a major security risk.
Choosing an MSP on price alone
Underspecified contracts routinely exclude HIPAA compliance work, 24/7 monitoring, and EHR-specific expertise. A low headline price often means critical capabilities are missing. Compare total scope, not just the monthly fee.
For a structured security and compliance review, Gart’s IT Audit Services identify exactly these patterns and provide a prioritized remediation roadmap — including a HIPAA audit preparation guide based on real enforcement findings.
Components of Managed IT Services for Healthcare
Data Security
Healthcare organizations face mounting challenges in protecting sensitive patient information from cyberattacks.
Many organizations mistakenly treat security as an afterthought, prioritizing functionality over safety. This approach is akin to building a boat and waterproofing it later—a strategy destined to fail. Another common misconception is over-reliance on third-party services, such as cloud providers, without addressing internal vulnerabilities.
Actionable Strategies for Enhanced Security
- Embed Security from Day One:
Organizations must design systems with security as a foundational element rather than an add-on. - Educate and Empower Teams:
Conduct regular training sessions to ensure all team members understand their roles in maintaining security. - Automate Security Processes:
Implement CI/CD pipelines integrated with testing tools to identify vulnerabilities with every code update. - Use Advanced Detection Systems:
Leverage intrusion detection and prevention tools to monitor and flag suspicious activities. - Exceed Regulatory Standards:
Compliance with standards like HIPAA is essential but represents the bare minimum. Organizations should proactively identify and address risks beyond what regulations require.
System Integration
- Seamless integration of EHRs, PMS, and diagnostic tools.
- Maintains interoperability between diverse systems.
Cloud Services
- Use secure cloud infrastructure for data access and telehealth delivery
- Meet HIPAA and GDPR standards with data placement and encryption
Compliance Management
- Monitor regulatory updates
- Provide documentation and audit readiness
- Support HITECH and global compliance frameworks
Managed IT Services vs. Break-Fix Model
| Aspect | Break-Fix Model | Managed IT Services |
| Approach | Reactive: Fixes issues as they arise. | Proactive: Prevents issues before they occur. |
| Cost | Unpredictable, pay-per-issue. | Fixed monthly fees. |
| Support | Limited to immediate problems. | Comprehensive, ongoing management. |
| Downtime | High due to lack of monitoring. | Minimal, thanks to proactive care. |
How to Choose a Managed IT Service Provider

To choose the best Managed IT Service Provider for your healthcare product, you should pay attention to several key factors.
1. Experience in Healthcare
Ensure the MSP understands the specific needs and regulations of the healthcare industry.
2. Proven Track Record
Look for client testimonials, case studies, and certifications like HIPAA compliance expertise. At Gart, our 5-star reviews and client testimonials reflect our commitment to excellence and our proven track record in the healthcare sector. Take a look at Clutch.
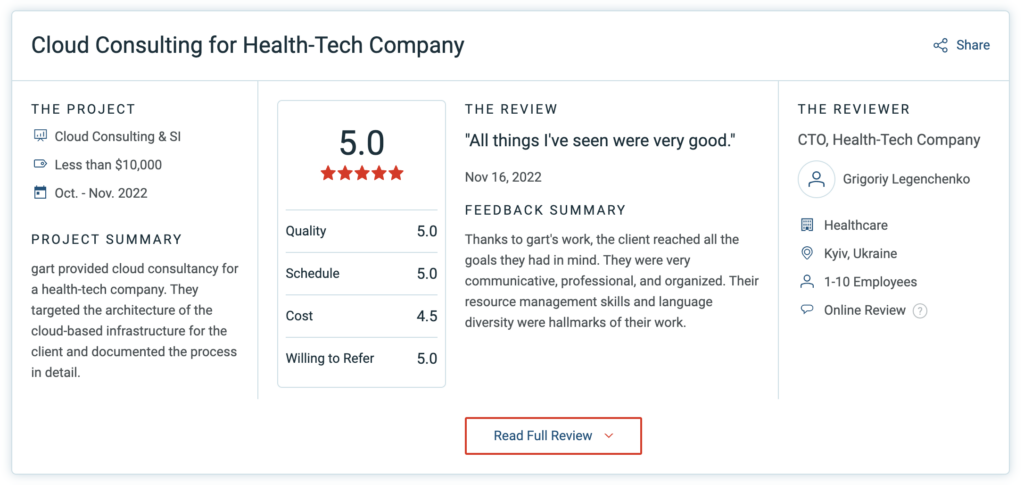
3. Scalability
Choose a provider that can grow with your practice.
Avoid one-size-fits-all approaches; your MSP should tailor services to your unique needs.
Read more: How to Choose a DevOps Provider for Your HealthTech Project
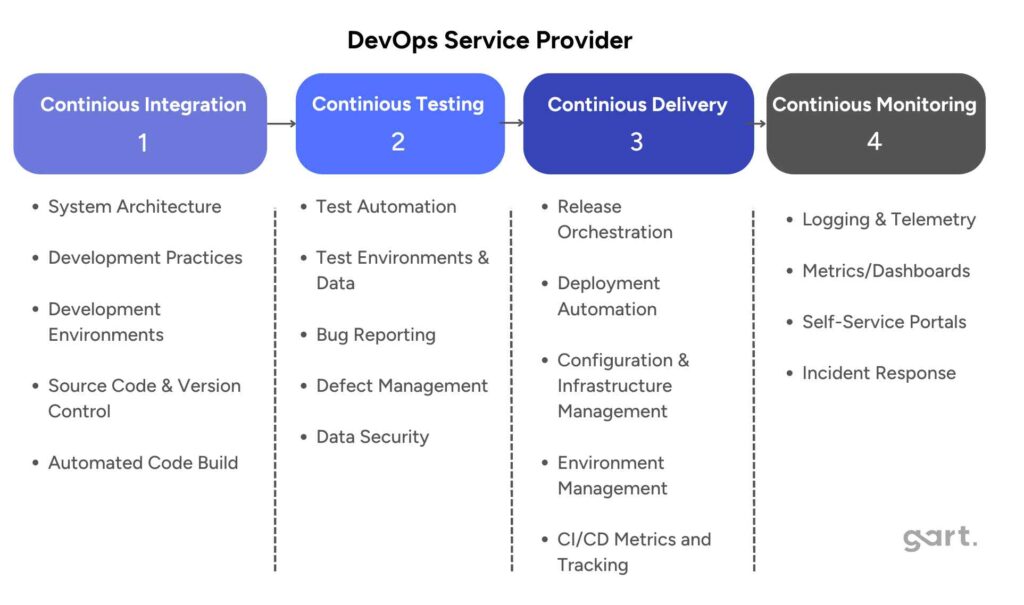
Read more: How to Choose a DevOps Provider for Your HealthTech Project — the same principles apply to MSP selection across regulated healthcare environments.
5 Key Takeaways for Healthcare Leaders Evaluating Managed IT Services
1. Managed IT is a strategic requirement, not an IT convenience
In a regulated, high-stakes environment, the question isn’t whether you can afford managed IT — it’s whether you can afford the exposure of not having it. HIPAA penalties, ransomware recovery costs, and the operational impact of unplanned downtime consistently exceed MSP investment by a wide margin.
2. Security and compliance must be built in from day one
GDPR, HIPAA, and HITECH compliance cannot be retrofitted into an architecture that wasn’t designed for them. Every infrastructure decision — cloud provider, access model, logging configuration — is a compliance decision in healthcare.
3. Proactive monitoring prevents incidents that reactive fixes cannot undo
A data breach cannot be “fixed” — only managed after the fact. The value of 24/7 monitoring is measured in the incidents that never occur and the audit findings that never appear, not just in faster ticket resolution.
4. Scalable IT infrastructure enables clinical growth without technology constraints
Adding a new location, expanding telehealth services, or acquiring a practice should be a clinical and business decision — not one constrained by IT capacity limits. A well-designed MSP model scales on demand.
5. The right MSP partnership frees clinical leadership to focus on care
Every hour a CMO or department head spends on an IT problem is an hour not spent on clinical strategy, staff, or patients. The operational value of that reallocation is real — and measurable.
Conclusion
Managed IT Services for Healthcare have moved decisively from optional infrastructure investment to a strategic operational requirement. The regulatory complexity of HIPAA, HITECH, and GDPR — combined with healthcare organizations’ status as the top target for ransomware groups — means that reactive, understaffed IT creates existential risk, not just operational inconvenience.
The organizations that navigate this landscape successfully share a common pattern: they partner with the right IT expertise early, before the breach, before the audit finding, before the system failure that delays a critical diagnosis. They treat IT not as a cost center to minimize but as a clinical enabler to invest in deliberately.
If you’re evaluating managed IT options for your healthcare organization, the right starting point is always a clear-eyed view of your current posture. Start with an IT audit— it’s the fastest way to understand what you actually need and build the internal case for investment with specifics, not assumptions.
For global interoperability standards and open-source healthcare IT tooling, the Linux Foundation‘s health initiatives provide valuable context on the direction the industry is moving — useful background for any organization planning a multi-year infrastructure strategy.
Ready to Build a Secure, HIPAA-Compliant IT Foundation?
Gart Solutions works with health-tech companies, hospitals, and digital health startups to deliver managed infrastructure, security, compliance, and DevOps — purpose-built for regulated healthcare. We’ve helped clients pass HIPAA audits, eliminate critical EHR downtime, migrate PHI to the cloud, and reduce IT costs by 30–40%.









