- Defining Cloud for Healthcare
- Why Cloud Computing in Healthcare Matters Now
- Cloud Deployment Models for Healthcare
- Key Benefits: What the Data Actually Shows
- Key Challenges in Cloud Adoption
- Healthcare Cloud Use Cases
- Compliance Deep-Dive: HIPAA, GDPR, and Beyond
- AWS vs Azure vs GCP in Healthcare
- Cloud Migration Roadmap for Hospitals
- Top 5 Mistakes Hospitals Make When Moving to Cloud
- Emerging Trends: AI, Zero Trust & Confidential Computing
- Cloud as a Disruptor in Healthcare IT
- Conclusion: The Future of Cloud in Healthcare
- Planning a Cloud Migration for Your Healthcare Organization?
The healthcare sector is gearing up for big changes, and cloud technology is quickly becoming a vital part of its IT backbone. As data demands grow and patient care and security needs become more complex, the cloud offers a scalable, efficient solution to improve healthcare operations.
Cloud computing in healthcare has crossed from a future aspiration to an operational baseline. Over 83% of healthcare organizations worldwide now use some form of cloud services, and the global market — valued at roughly $75 billion in 2026 — is growing at a 17% annual rate, on track to surpass $312 billion by 2035.
Yet many healthcare IT leaders still operate on partial, surface-level implementations — hosting some workloads in cloud while keeping the rest on aging on-premise systems, often without a coherent compliance or cost strategy. This guide addresses that gap directly.
What you’ll find here is not a generic overview. It’s a practitioner’s resource built on real migration projects, compliance architecture patterns, and honest vendor comparisons — the kind of content that helps you make decisions, not just understand concepts.
Defining Cloud for Healthcare
“A cloud-based architecture can help overcome many of these challenges, turning IT from a backend support function into a strategic enabler of healthcare.”
Jason Jones
The term “cloud” is often associated with innovation but also confusion, as various industries interpret it differently. In healthcare, cloud computing refers to delivering IT services—storage, applications, and networking — through remote servers rather than traditional on-premise systems.
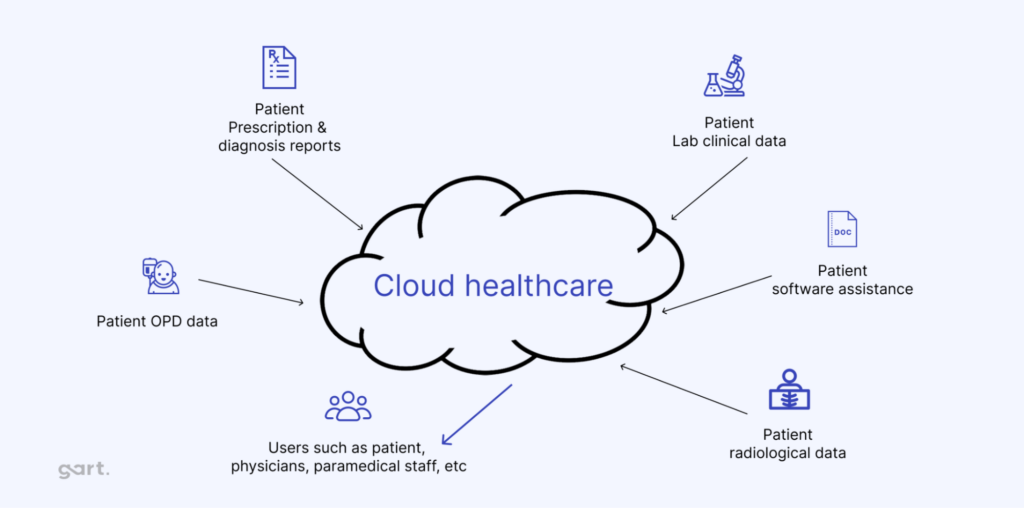
- Private Cloud: internal infrastructure managed by an organization.
- Public Cloud: external services, e.g., AWS, Azure, offering flexible, on-demand resources but with security considerations.
- Hybrid Cloud: combination of private and public, enabling flexible use for storage, scalability, and backup.
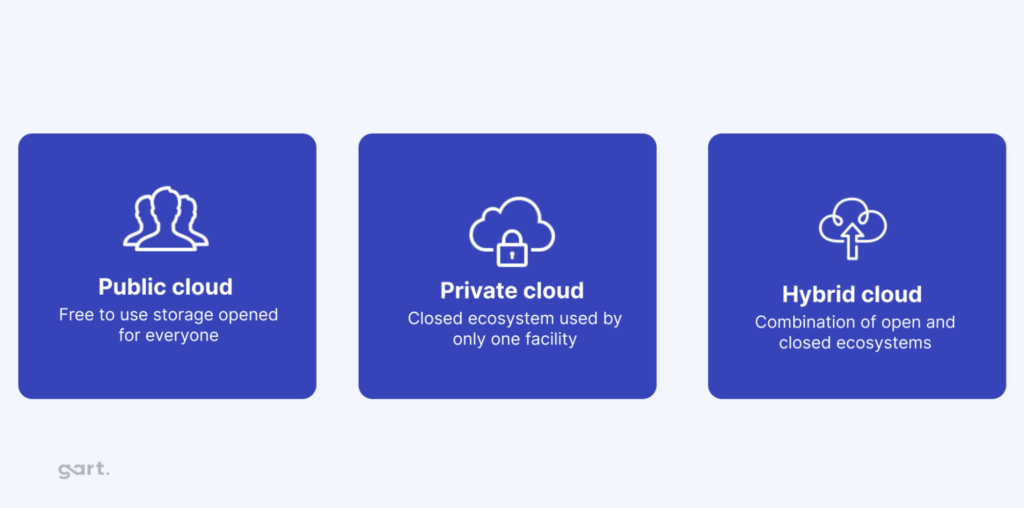
Cloud technology can be configured in several ways to meet the specific needs of healthcare providers:
Private Cloud
Managed internally within the organization, a private cloud offers control and security for sensitive healthcare data, ensuring that resources are exclusively used by the organization.
Public Cloud
“In healthcare, especially, we need systems that are horizontally and infinitely scalable based on organizational needs.”
Tony Nunes, Pharmacoepidemiologist, Assistant Professor
Hosted by third-party providers like AWS or Microsoft Azure, public clouds offer scalable resources on demand, though concerns about data privacy and security often restrict their use for healthcare’s most sensitive information.
Hybrid Cloud
“The hybrid cloud approach really has become something that’s evolving to a point where today, a majority of healthcare providers…are looking to balance between an on-prem private cloud solution and a hybrid cloud public workload solution.”
Chris Mohen
Combining private and public cloud, a hybrid model provides flexibility by allowing healthcare providers to scale with external resources while maintaining strict control over critical data.
For healthcare, the hybrid cloud often represents an ideal balance, offering an adaptable infrastructure that aligns with data privacy regulations while providing scalability. Steven Lazer, CTO of Healthcare at Dell EMC, suggests that healthcare has essentially been engaging in cloud practices for years under different labels, such as affiliate services, where remote access was given to necessary services
Lazer advocates for a “cloud-smart” approach, where healthcare organizations strategically place applications in the cloud or on-premises based on each application’s unique needs. This model enhances flexibility, scalability, and data security while supporting both traditional and emerging healthcare needs.
Why Cloud Computing in Healthcare Matters Now
Several forces are converging in 2026 to make cloud adoption not just beneficial but structurally necessary for healthcare organizations:
Data volume explosion. Global healthcare data is projected to exceed 2,000 exabytes. Legacy on-premise infrastructure was never designed to handle this. Imaging alone — representing 80–85% of a hospital’s total stored data — creates storage demands that simply cannot be met cost-effectively without cloud-scale infrastructure.
AI and real-time analytics requirements. Clinical AI — from diagnostic imaging models to sepsis prediction — requires the kind of elastic compute capacity that only public or hybrid cloud can deliver. Running these workloads on-premise means either prohibitive hardware investment or accepting that AI will remain a pilot program, never reaching production.
Telehealth is permanent infrastructure. Behavioral health telehealth adoption reached a 93% adoption rate by 2024, and over 30 million patients now use remote monitoring systems. These services run on cloud. Organizations without cloud infrastructure cannot reliably deliver them at scale.
Financial pressure on IT budgets. Healthcare margins compressed significantly post-pandemic. Cloud’s pay-as-you-go model — combined with the elimination of hardware refresh cycles — delivers a tangible cost structure advantage over traditional data center operations for most workloads.
Cloud Deployment Models for Healthcare
Healthcare’s regulatory and operational requirements make deployment model selection genuinely consequential — not just a technical preference. Here is how each model performs against the criteria that matter most to healthcare organizations:
| Model | Control | Scalability | Cost Structure | Best For |
|---|---|---|---|---|
| Private Cloud | Highest | Limited — bounded by owned hardware | High CapEx; predictable OpEx | Highly regulated data; organizations with existing data center investment |
| Public Cloud (AWS, Azure, GCP) | Shared responsibility | Elastic — scale on demand | Low CapEx; variable OpEx | Analytics, AI workloads, telehealth, dev/test environments |
| Hybrid Cloud | Configurable per workload | High — burst to public cloud | Balanced; architecture-dependent | Most mid-to-large healthcare organizations; regulatory flexibility |
| Multi-Cloud | Distributed | Highest | Complex — requires FinOps discipline | Large health systems with diverse workload needs; vendor risk mitigation |
In practice, the hybrid model dominates healthcare adoption. It lets organizations maintain strict control over PHI (Protected Health Information) in a private environment while using public cloud capacity for analytics, backup, and scalable patient-facing applications. Public cloud deployments captured about 42% of the market in 2025, while hybrid is the fastest-growing segment at an 18.2% CAGR through 2032 — reflecting exactly this pattern.
“The hybrid cloud approach has become something that’s evolving to a point where today, a majority of healthcare providers are looking to balance between an on-prem private cloud solution and a hybrid cloud public workload solution.”— Chris Mohen, Healthcare IT Leader
Key Benefits: What the Data Actually Shows
Generic benefit lists (“improved scalability,” “cost savings”) are not useful for decision-making. The table below maps each benefit category to a concrete metric from real healthcare deployments:
| Benefit Area | Mechanism | Real-World Metric |
|---|---|---|
| Cost Reduction | Eliminate hardware refresh, consolidate data centers, use elastic capacity | 15–30% reduction in IT operational costs; up to 40% lower administrative overhead |
| Deployment Speed | CI/CD pipelines, containerized environments, infrastructure-as-code | Deployment cycles reduced from days to hours (Gart client case study) |
| Readmission Reduction | IoT remote monitoring + cloud-based analytics trigger early interventions | Up to 38% reduction in 30-day readmission rates in documented programs |
| Disaster Recovery | Cloud-native backup, geo-redundant storage, automated failover | RTO reduced from hours to minutes for cloud-native architectures |
| Compliance Posture | Built-in audit trails, encryption at rest and in transit, IAM controls | Audit preparation time reduced by 60%+ when using HIPAA-ready cloud frameworks |
| AI Enablement | Elastic GPU compute for model training and inference | Diagnostic AI models deployed in days vs months with cloud-native MLOps pipelines |
“As a CFO, I no longer am over-investing in our IT environments. Cloud has allowed us to consolidate and use only what is needed, without pools of unused storage or compute capacity.”— Tony Nunes, Pharmacoepidemiologist & Healthcare IT Leader (22+ years)
Key Challenges in Cloud Adoption
Despite the clear benefits, healthcare’s journey to the cloud is marked by challenges that require careful planning and robust solutions:
Data Privacy and Security
Healthcare data is a prime target for cyberattacks, so security is essential. Although cloud providers offer strong protections, healthcare organizations must ensure strict access controls and encryption to comply with regulations like HIPAA.

Legislations related to Cloud security and healthcare:
| Legal Requirements | Privacy & Data Protection | Cybersecurity | Cloud Security | Health |
|---|---|---|---|---|
| EU | – General Data Protection Regulation (GDPR) | – Network and Information Security Directive (NIS Directive) | – None | – Medical Device Regulation (MDR) |
| – European Union Cybersecurity Act | – Electronic Cross-Border Health Services Directive | |||
| – Medical Device Directive (MDD) | ||||
| National | – National data protection or privacy laws | – National information and data security laws | – National cloud security laws | – National healthcare-related laws for data protection and cybersecurity |
Security remains a paramount concern as healthcare organizations adopt cloud technologies:
- Data Encryption: Both symmetric and asymmetric encryption methods are essential to secure data at rest and in transit.
- Access Controls: Multi-factor authentication and role-based access control ensure that only authorized personnel can access sensitive patient information.
- Compliance with Regulations: Healthcare organizations must comply with frameworks such as HIPAA in the U.S., GDPR in Europe, and local privacy laws. Ensuring compliance helps mitigate risks associated with data breaches.
- Continuous Monitoring: Tools such as Intrusion Detection Systems (IDS) and Security Information and Event Management (SIEM) platforms are vital for identifying and responding to threats in real-time.
Costs
Setting up and managing a cloud environment can be expensive, especially for hybrid models. But as bandwidth costs drop and security improves, the long-term gains in efficiency and scalability are making cloud solutions more affordable.
“As a CFO, I no longer am over-investing in our IT environments… Cloud has allowed us to consolidate and use only what is needed, without pools of unused storage or compute capacity.”
Tony Nunes
Resistance to Change
Switching to cloud disrupts traditional IT roles, needing collaboration between IT and clinical teams. This shift requires cultural adjustments to align data access with security needs.
The bigger challenge isn’t technology—we can solve a lot of problems with technology—but rather, it’s the people and the process.
Jason Jones
Knowledge Gaps
Some organizations hesitate to adopt cloud tech due to limited understanding of how it integrates or improves their current systems. Demonstrating real-world successes can help show the cloud’s potential.
Dan Trott, a healthcare strategist with Dell EMC, highlights that while security used to be the foremost concern, now the greatest obstacle is educating stakeholders on how cloud solutions healthcare can work for them and how they can maximize cloud-based resources for better outcomes.
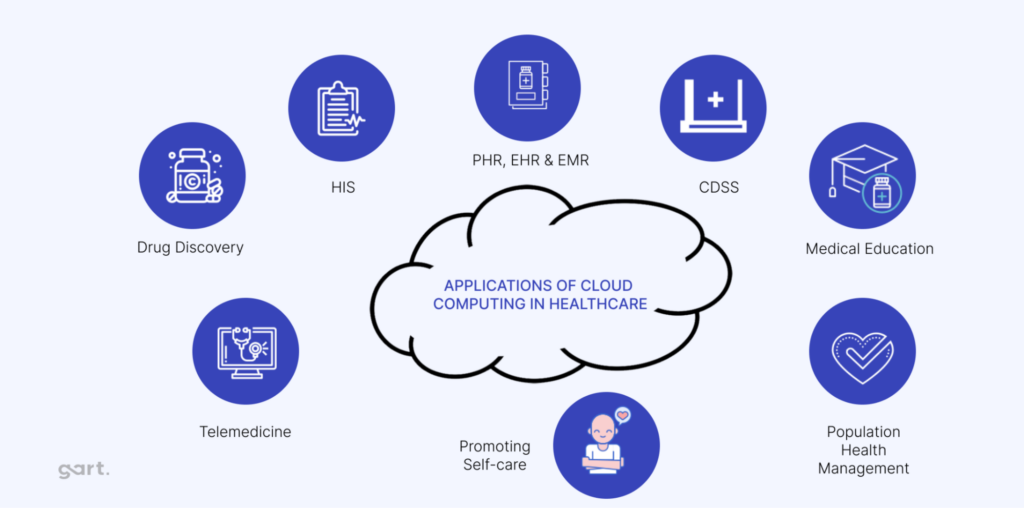
Healthcare Cloud Use Cases
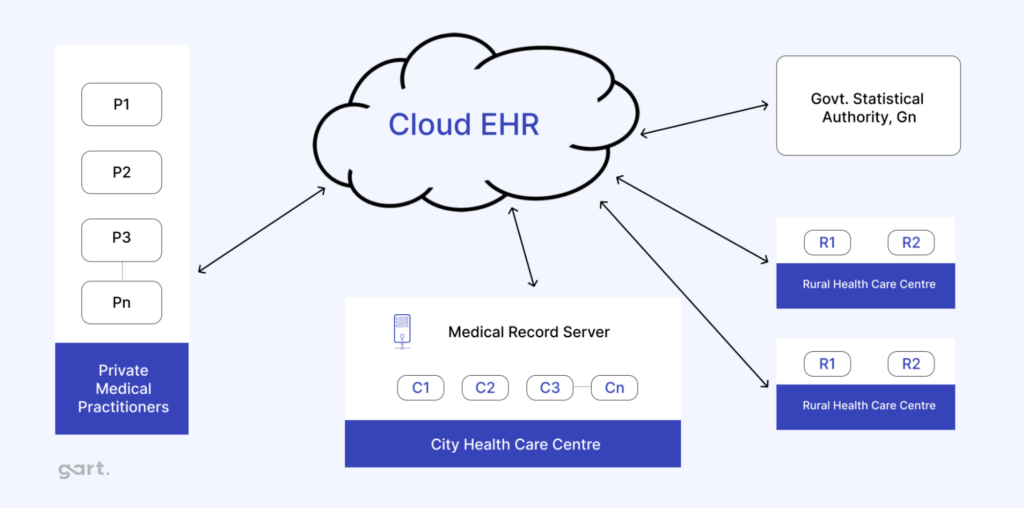
The potential applications for cloud in healthcare are vast, ranging from managing data-heavy imaging systems to electronic health records (EHRs) and research initiatives.
- Electronic Health Records (EHRs): Cloud-based EHRs enable seamless sharing of patient data among healthcare providers. Advanced encryption and access controls ensure data privacy and security.
- Telemedicine and Remote Monitoring: Cloud technologies facilitate remote consultations and monitoring, expanding healthcare access in underserved regions. For instance, blockchain-based models enhance secure data sharing in telemedicine platforms.
- Health Management and Predictions: Predictive analytics powered by cloud computing aids in identifying health trends and managing chronic diseases. Machine learning algorithms on cloud platforms have been used for mortality predictions and early disease detection.
- Medical Imaging and Diagnostics: Cloud platforms allow the storage and analysis of high-resolution imaging data, enabling faster and more accurate diagnoses.
- Collaboration and Research: Cloud services enable collaboration across healthcare providers, enhancing clinical research and innovation. Centralized platforms support multi-disciplinary teams in analyzing data efficiently.
Patient Population Analysis with Cloud Computing
Cloud computing revolutionizes patient population analysis by providing robust tools for aggregating, processing, and analyzing vast datasets from diverse demographics. Through centralized storage of electronic health records (EHRs), patient demographics, and social determinants of health, cloud platforms enable healthcare providers to identify disease patterns, predict outbreaks, and design targeted public health interventions. Advanced analytics tools hosted on cloud platforms, combined with real-time data from Internet of Things (IoT) devices, allow healthcare systems to monitor patient vitals and derive insights at scale.
The integration of Container as a Service (CaaS) and Continuous Integration/Continuous Deployment (CI/CD) pipelines further enhances population health analytics. CaaS enables the deployment and scaling of containerized applications, allowing healthcare organizations to run complex analytics tools and machine learning models efficiently. CI/CD ensures these applications are continuously updated and refined, fostering innovation and reducing downtime for critical services. For instance, a population health model can seamlessly incorporate new data sources or algorithm improvements without disrupting operations.
Moreover, cloud platforms promote interoperability, consolidating data from clinics, laboratories, and pharmacies into a unified system. This integrated approach helps address disparities in healthcare delivery by enabling targeted interventions in underserved populations. Security measures, such as encryption and pseudonymization, ensure patient privacy while permitting researchers and policymakers to access de-identified datasets for broader health studies. By leveraging CaaS and CI/CD alongside cloud computing, healthcare systems can transition from reactive to proactive care strategies, improving public health outcomes with greater agility and efficiency.
Medical Imaging
“Medical imaging represents 80-85% of the total amount of data any one hospital has to manage and store.”
Dan Trott
Medical imaging is essential in healthcare, helping doctors diagnose, plan treatments, and monitor progress. As imaging tech has advanced, so has the size and complexity of imaging data, creating new challenges around storage, access, and security.
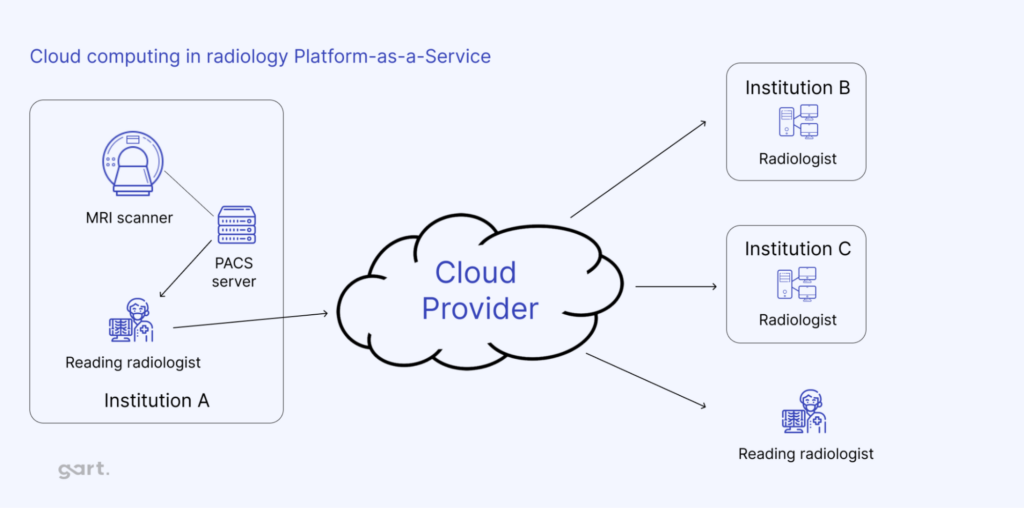
Here’s how cloud storage is transforming medical imaging:
Easier Storage & Scalability
Cloud storage handles large amounts of imaging data without the need for physical hardware. This scalability is especially helpful for smaller facilities that don’t want to invest in new servers as data needs grow.
Better Security & Compliance
Leading cloud providers offer strong security, like encryption and multi-factor authentication, often surpassing what on-site systems can do. These solutions are designed to meet healthcare regulations, making compliance easier.
Improved Data Sharing & Collaboration
Cloud-based imaging supports easy data sharing across healthcare facilities, which is crucial for patients seeing multiple providers. This ensures every provider has access to the same, up-to-date images.
Disaster Recovery & Backup
Cloud solutions automatically back up imaging data across locations, protecting against data loss from hardware failures or natural disasters.
Fast Image Access
Storing images in the cloud allows providers to access them instantly from anywhere, which is especially valuable in emergencies when quick access can impact patient outcomes.
Electronic Health Records (EHR)
Electronic Health Records (EHRs) are digital versions of patient charts and are a key part of modern healthcare. Unlike paper records, EHRs provide a complete, real-time, and secure way to manage patient information across different healthcare settings.
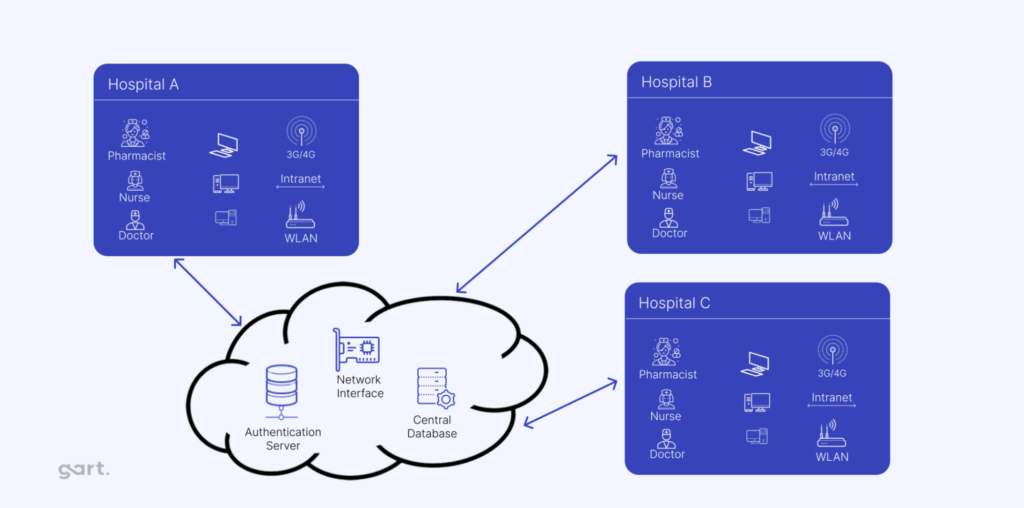
Using the cloud to store and manage EHRs is a big step forward, though it’s complicated by strict privacy laws and the need for strong security. While some providers offer hosted models, fully cloud-based EHR solutions are still a challenge due to the sensitivity of patient data. Here’s how cloud technology is helping to advance EHRs:
Scalability and Cost-Effectiveness
Cloud-based EHRs are more affordable and scalable, making them ideal for smaller practices and rural healthcare providers. By storing data in the cloud, organizations can reduce physical storage needs and avoid the high costs of running their own servers and data centers.
Improved Data Sharing and Interoperability
Cloud systems allow data to be accessed from anywhere, supporting better interoperability across healthcare facilities. This enables patient data to follow the patient through different providers, ensuring consistent care no matter the location.
“What the cloud provides is a way of outsourcing that information… putting it into a very large data center that has significant cost efficiency and volume efficiency.”
Dan Trott
Enhanced Data Security
Many cloud providers offer top-level security features like encryption, multi-factor authentication, and real-time monitoring. These protections often go beyond what traditional on-site systems provide, addressing security concerns while meeting healthcare regulations.
Automatic Updates and Maintenance
Cloud-based EHR providers handle system updates and maintenance, so healthcare providers always have the latest security and functionality enhancements without disrupting their workflow. This is especially helpful for organizations without dedicated IT resources.
Disaster Recovery and Data Backup
Cloud storage includes built-in data backup and disaster recovery options, meaning patient information stays safe even if there’s a hardware failure or natural disaster. This added redundancy is essential for protecting patient data and keeping services running smoothly.
Clinical Research and Development
A cloud-based infrastructure is valuable for research-intensive organizations as it allows researchers to quickly scale resources for data processing. Data silos can be eliminated, providing a more seamless research process and helping projects launch faster. For instance, grants often require complex data environments, which can be set up more efficiently in a cloud environment.
These use cases demonstrate how the cloud supports efficiency and innovation by reducing physical storage needs and enhancing data security.
Compliance Deep-Dive: HIPAA, GDPR, and Beyond
Compliance in healthcare cloud is not a single certification — it is a continuously maintained architecture posture. The table below outlines the frameworks most relevant to healthcare cloud deployments and their practical implications for architecture decisions:
| Framework | Scope | Key Architecture Requirements |
|---|---|---|
| HIPAA | US — PHI protection | Encryption at rest and in transit; access controls; audit logs; BAAs with cloud vendors; breach notification within 60 days |
| HITECH Act | US — EHR data | Meaningful use of health IT; HIPAA-compliant apps are HITECH compliant — aligns your obligations |
| GDPR | EU — all personal data including health records | Data minimization; consent management; right to erasure; data residency within EU for EU citizen data; DPA agreements |
| ISO 27001 | Global — information security | Risk assessment framework; security controls; continuous monitoring; required by many enterprise healthcare buyers for vendor qualification |
| HL7 FHIR | Global — interoperability standard | API-first data exchange between systems; increasingly mandated for payer data sharing in the US |
| PIPEDA | Canada — personal data | Consent for data collection; data accuracy; safeguards for personal information; closely aligned with GDPR |
💡 Practical note: HIPAA-compliant architecture is also HITECH compliant. PIPEDA compliance typically maps well to GDPR requirements. If you are building for US + EU + Canada simultaneously, design to GDPR/ISO 27001 standards first — you will satisfy the others more efficiently.
AWS vs Azure vs GCP in Healthcare
Healthcare organizations frequently ask which cloud provider is best. The honest answer is that there is no universal winner — the right platform depends on your existing technology stack, geographic requirements, and specific workload profile. Here is a practical comparison based on real deployment patterns:
| Criteria | AWS | Microsoft Azure | Google Cloud (GCP) |
|---|---|---|---|
| HIPAA BAA | Available; broad service coverage | Available; deep Microsoft 365 integration | Available; HIPAA-eligible services documented |
| GDPR Compliance | EU data residency options | Strong EU presence, dedicated EU data boundary | EU data residency options |
| EHR Integration | Strong with AWS HealthLake (FHIR-native) | Strong with Azure Health Data Services + Epic/Cerner partnerships | Google Cloud Healthcare API (FHIR, HL7v2, DICOM) |
| Medical Imaging / DICOM | Amazon HealthImaging — purpose-built | Azure API for DICOM — mature | Cloud Healthcare API includes DICOM support |
| AI / ML Workloads | SageMaker — mature MLOps; largest model marketplace | Azure OpenAI integration; Copilot ecosystem; strong for .NET stacks | Vertex AI; strongest for organizations already using Google Workspace |
| Best For | Greenfield healthcare SaaS; data-heavy workloads; startups | Organizations with Microsoft stack (Office 365, Active Directory, .NET apps) | Analytics-heavy workloads; organizations using Google Workspace |
| Typical Cost Pattern | Most competitive for compute; storage pricing requires optimization | Significant savings if you have existing Microsoft licensing (hybrid benefit) | Competitive sustained use discounts; strong for BigQuery analytics workloads |
💡 Cost reality check: A mid-size hospital system (500 beds) migrating EHR and imaging workloads can expect first-year cloud spend of $600K–$1.2M depending on architecture choices, data volumes, and existing vendor agreements. The breakeven against on-premise infrastructure typically occurs in year 2–3, with ongoing savings accelerating as workloads are optimized. Organizations that skip FinOps discipline in year 1 often see costs 40–60% above initial estimates.
Cloud Migration Roadmap for Hospitals
The following roadmap is based on patterns from real healthcare cloud migration projects. It is designed to minimize compliance risk while delivering measurable value at each phase:
1. Infrastructure & Compliance Audit (Months 1–2)
Map all existing systems, data flows, and PHI touchpoints. Identify compliance gaps against HIPAA/GDPR/applicable frameworks. Assess current security posture, vendor contracts, and migration blockers. This audit defines the actual migration scope — organizations that skip it consistently underestimate complexity and cost.
2. Architecture Design & Vendor Selection (Months 2–3)
Select cloud provider(s) based on workload profile and existing stack. Design HIPAA-compliant architecture with encryption, IAM, audit trails, and data residency controls built in from the start. Execute BAA agreements. Define the deployment model (hybrid is most common at this stage).
3. Foundation Build & Security Controls (Months 3–5)
Deploy cloud landing zone with security controls active from day one. Implement MFA, RBAC, VPN/private connectivity, encryption, and continuous monitoring infrastructure. Set up CI/CD pipelines for infrastructure-as-code. Establish FinOps visibility before spending scales.
4. Non-Critical Workload Migration (Months 4–8)
Begin with lower-risk workloads: dev/test environments, analytics, backup, administrative systems. Build team confidence and operational processes. Identify integration issues before migrating clinical systems. Pilot remote monitoring or telehealth on cloud infrastructure.
5. Clinical System Migration (Months 6–14)
Migrate EHR, PACS, and clinical applications with parallel-run periods. Use phased cutover, not big-bang replacement. Validate compliance at each milestone. Ensure clinical staff training is completed before cutover — not after. Document all compliance evidence for audit readiness.
6. Optimize & Scale (Months 12+)
Continuous cost optimization via FinOps practices. Expand AI and analytics workloads using cloud-native services. Regular compliance audits and penetration testing. Expand hybrid cloud capabilities as workload patterns become established.
Top 5 Mistakes Hospitals Make When Moving to Cloud
Based on patterns observed across healthcare cloud projects, these are the failure modes that consistently derail migrations and inflate costs:
- Treating security and compliance as a final step, not a foundation. Organizations that design their cloud architecture first and layer compliance on afterward create structural problems that are expensive to fix. HIPAA-compliant encryption, IAM, and audit trail architecture must be designed in from the first infrastructure decision.
- Attempting a big-bang migration of clinical systems. Replacing all clinical systems simultaneously is among the highest-risk patterns in healthcare IT. The standard that works is: pilot with non-clinical workloads, build operational muscle, then migrate clinical systems in phases with parallel-run periods.
- Underinvesting in FinOps from day one. Cloud costs are highly architecture-sensitive. Without tagging policies, budget alerts, and a designated FinOps function, healthcare organizations routinely overspend by 40–60% in the first 18 months. Visibility into cloud spend should be established before migration begins.
- Treating cloud migration as an IT project, not a clinical change management initiative. Clinical staff who do not understand or trust new systems find workarounds. The most technically excellent EHR migration fails if nurses are keeping parallel paper records because the cloud interface is unfamiliar. Change management investment must match technology investment.
- Not executing BAA agreements with all cloud vendors before handling PHI. A Business Associate Agreement is a legal prerequisite under HIPAA — not a formality. Organizations that move PHI to cloud environments without executed BAAs are in immediate violation, regardless of the underlying technical security of the implementation.
Emerging Trends: AI, Zero Trust & Confidential Computing
Cloud computing in healthcare is a rapidly evolving domain. The following developments will materially affect how healthcare IT leaders make architecture decisions in the next 2–3 years:
AI-Native Healthcare Cloud
Cloud providers are building healthcare-specific AI services directly into their platforms. Oracle Health launched an AI Center of Excellence for healthcare in September 2025. Anthropic launched Claude for Healthcare in January 2026 — a HIPAA-ready product specifically built for healthcare providers, payers, and health tech companies. The trend is toward AI services that are compliance-ready by default, reducing the integration overhead for healthcare organizations.
Zero Trust Architecture
The traditional perimeter security model — where everything inside the network is trusted — is structurally incompatible with cloud and hybrid environments. Zero Trust operates on the principle of “never trust, always verify” — every access request is authenticated and authorized regardless of network location. For healthcare, where staff access PHI from clinical workstations, personal devices, and remote locations simultaneously, Zero Trust is becoming the mandatory security architecture rather than an advanced option.
Confidential Computing
Confidential computing secures data during processing — not just at rest and in transit — by performing computations within hardware-protected enclaves. This enables healthcare organizations to run analytics on sensitive patient data without exposing it to the underlying cloud infrastructure, opening new possibilities for multi-organization research collaborations that were previously impossible due to privacy constraints.
Edge Computing + Cloud
IoT medical devices in ICUs, operating rooms, and remote patient monitoring programs generate data that cannot always be sent to central cloud for processing due to latency requirements. Edge computing processes this data locally and sends results — not raw data — to cloud platforms. This architecture is becoming standard for real-time clinical monitoring systems.
Hybrid Cloud Growth
Hybrid cloud is the fastest-growing deployment model in healthcare at an 18.2% CAGR through 2032. This reflects the reality that most healthcare organizations will maintain on-premise systems for at least some workloads — either due to regulatory requirements, existing infrastructure investment, or specific clinical applications — while scaling cloud for new workloads and analytics.
Cloud as a Disruptor in Healthcare IT
The move to cloud computing is shaking up healthcare IT and redefining traditional roles. With the cloud, healthcare providers can use “bimodal IT,” where stable systems work alongside fast, DevOps-driven setups. This approach meets both steady operational needs and the quick-paced demands of data-driven patient care.
“This concept of ‘bimodal IT’ — where you can use infrastructure in a consolidated way while still delivering essential services — really enables healthcare to enhance the quality and value of the care system.”
Steven Lazer
Changing IT Roles
Cloud computing in healthcare pushes IT teams to move from specialized, separate roles (like storage or security) to a more service-oriented and collaborative approach. This shift brings IT closer to clinical workflows, enabling faster data sharing and quicker response times for patient care.
Cost Savings
Consolidating IT into unified cloud platforms cuts down on “maintenance-only” spending. For example, Dell EMC estimates significant cost reductions when switching to cloud systems, allowing more resources to go toward innovative patient care solutions.
Delivering Higher Value
With cloud solutions, healthcare IT can focus on real impact rather than routine tasks. For example, a developer environment can be set up and taken down in just 48 hours, allowing rapid innovation while keeping resources directed at high-impact areas.
“The next step of evolution we’re going to see in cloud is around the concept of a virtual private cloud—using shared infrastructure but isolated resources.“
Steven Lazer
Мirtual private clouds are the next phase, where organizations can gain the scalability benefits of public cloud while maintaining the security of private cloud through isolated resources on shared infrastructure.
Cloud computing in healthcare is rapidly evolving, with emerging technologies enhancing its capabilities:
- Zero Trust Architecture: Adopting a Zero Trust model ensures no implicit trust for any user or system, enhancing security in cloud environments.
- AI and Machine Learning: Real-time threat detection and advanced predictive models are becoming integral to healthcare cloud solutions.
- Blockchain Integration: Blockchain provides decentralized and immutable data storage, enhancing trust and transparency in healthcare operations.
- Confidential Computing: Techniques to secure data during processing are gaining traction, enabling sensitive operations without exposing data to risks.
Cloud is disrupting the old IT model, building a fast, scalable, and integrated infrastructure that directly supports better care delivery.
Conclusion: The Future of Cloud in Healthcare
“Cloud really becomes a disruptor of the status quo within IT.“
Tony Nunes
As healthcare organizations continue adopting cloud solutions, they are poised to deliver more reliable, efficient, and scalable services to patients. The cloud enables them to break free from traditional IT limitations, reduce costs, enhance data security, and improve operational resilience. As demonstrated by the success at Wake Forest Baptist Medical Center and other institutions, healthcare is ready to move into a new era where the cloud not only supports IT but also becomes integral to patient-centered care and operational excellence.
Through a thoughtful approach to cloud adoption, healthcare organizations can unlock new potential for innovation, efficiency, and patient satisfaction, transforming how care is delivered in a digitally connected world.
The following experts contributed valuable insights and perspectives, which were instrumental in the creation of this article:
- Tony Nunes: 22+ years in healthcare IT.
- Chris Mohen: Experience in clinical areas and transformative IT solutions.
- Steven Lazer: Global Healthcare & Life Sciences CTO – Dell Technologies at Dell Technologies
- Jason Jones: 15+ years, focusing on cloud strategies for healthcare.
- Dan Trott: Extensive experience since 2010, working with clinical and IT solutions.
Planning a Cloud Migration for Your Healthcare Organization?
Gart Solutions has delivered HIPAA-compliant cloud migrations, DevOps transformations, and ISO 27001 certifications for health tech companies globally. We deliver quick wins from day one — and a compliance architecture built to last.
Cloud Migration
AWS, Azure, GCP — HIPAA-compliant by design
DevOps & CI/CD
Automate deployments, reduce downtime
IT Audit & Compliance
HIPAA, ISO 27001, GDPR readiness
Infrastructure Management
Managed services, SRE, monitoring
Fractional CTO
Strategic tech leadership for scaling
Digital Transformation
End-to-end strategy & execution
See how we can help to overcome your challenges









