What is Digital Transformation in Healthcare?
Digital transformation in healthcare is no longer a future trend — it is the operational baseline for organizations that want to survive and lead in 2026.
Digital transformation in healthcare refers to the systematic integration of digital technologies — AI, cloud infrastructure, IoT, telemedicine, electronic health records (EHR), robotics, and advanced analytics — into every dimension of healthcare delivery, management, and operations.
It goes far beyond swapping paper for screens. A genuine digital transformation rethinks how hospitals, clinics, labs, and insurers create value for patients and how they collaborate across the entire care continuum.
Simple definition: Digital transformation in healthcare means using technology to fundamentally improve how care is delivered, experienced, and paid for — not just digitizing existing processes, but redesigning them from the ground up.
This guide breaks down 10 real implementation cases, the most common challenges, measurable benefits, and a practical roadmap for healthcare leaders.
Why Is It Gaining Momentum Now?
Several converging forces accelerated healthcare digitization well beyond the COVID-19 period:
Rising patient expectations:Patients compare healthcare to their experience with Amazon or Netflix and demand convenience, personalization, and instant access to their data.
Technology maturity:AI, large language models, and IoT devices reached production-grade reliability that makes large-scale healthcare deployment viable.
Financial pressure:Hospital margins compressed significantly post-pandemic. Automation and digital workflows are now a profitability lever, not a luxury.
Regulatory mandates:Governments from the US to the EU now require interoperable digital health records, telemedicine reimbursement frameworks, and mandatory data security standards.
Workforce shortages:With over 10 million unfilled healthcare roles globally projected by 2030 (WHO), automation and AI-assisted care are becoming a workforce strategy.
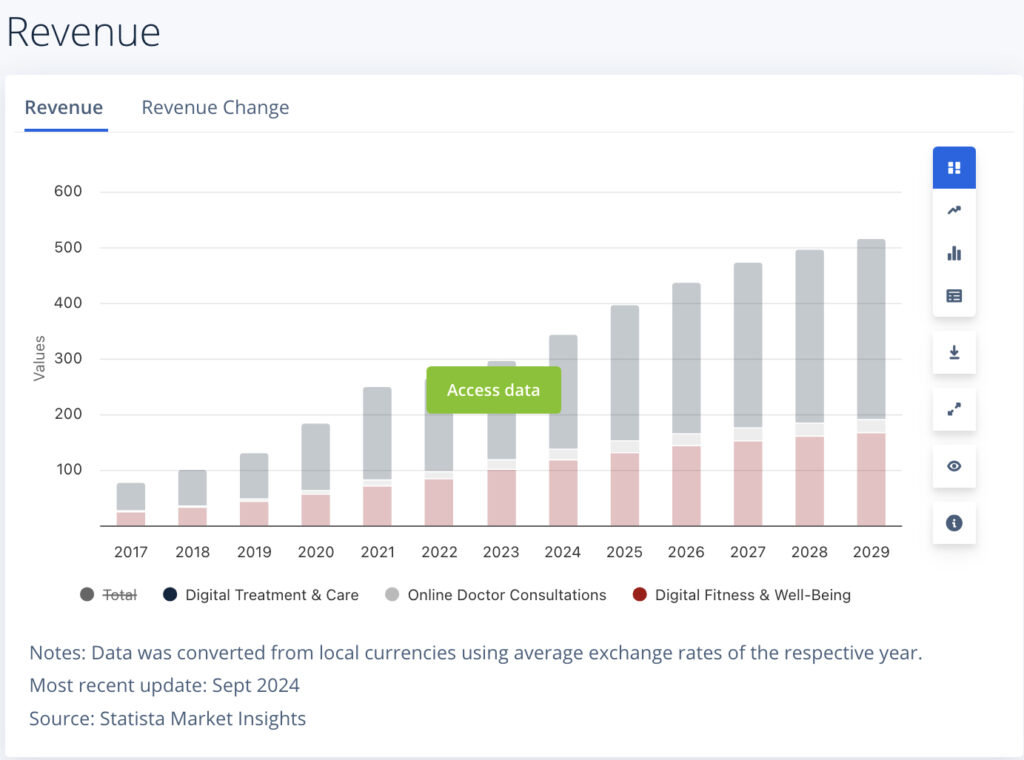
A Statista report projects the global digital healthcare market to reach $504.4 billion by 2025, underscoring how essential digital transformation has become for competitive and efficient healthcare delivery.
88% of healthcare technology leaders prioritize improving the patient experience in their investments (according to a Deloitte survey)
This shift underscores the necessity for healthcare professionals, including doctors, nurses, and administrative staff, to stay abreast of ongoing digital advancements.
Key Drivers of Digital Transformation in Healthcare (2026)
Artificial Intelligence
AI has crossed from experimental to mission-critical in healthcare. Today it powers:
Automated clinical documentation that reduces physician burnout
Diagnostic imaging analysis for radiology, pathology, and ophthalmology with accuracy matching or exceeding specialists
Predictive risk scoring for sepsis, cardiac events, and readmission prevention
AI-powered triage chatbots that handle over 30% of patient inquiries without human escalation
Drug discovery acceleration through molecular simulation (reducing timelines from years to months)
Google DeepMind's AlphaFold resolved a 50-year protein-folding problem, and its healthcare applications now inform drug design globally — a concrete proof point that AI delivers transformative, not incremental, value.
Internet of Things (IoT) in Healthcare
The number of connected medical devices globally exceeded 500 million in 2025. These devices enable:
Continuous remote patient monitoring for chronic conditions, reducing hospital admissions by up to 38%
Smart hospital infrastructure (asset tracking, bed management, HVAC optimization)
Wearable biosensors detecting arrhythmias, hypoglycemia, and medication adherence in real time
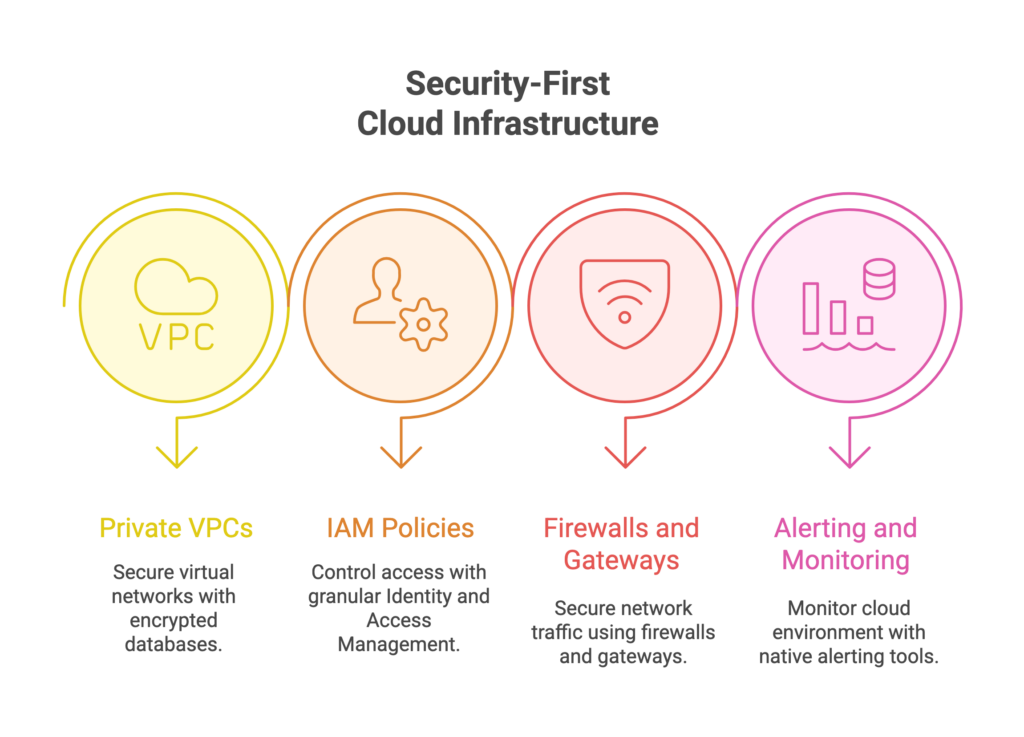
Cloud Infrastructure
Modern healthcare digital transformation runs on HIPAA-compliant cloud platforms. Cloud enables scalable data storage, real-time analytics, disaster recovery, and the computational power required for AI workloads — without the capital cost of on-premise data centers.
Robotics and Automation
Beyond the well-known da Vinci Surgical System, robotics now extends to hospital logistics (automated medication dispensing, supply chain robots), rehabilitation (exoskeletons), and AI-assisted clinical decision support that automates protocol-driven care decisions.
Measurable Benefits of Digital Transformation in Healthcare
The audit of this content flagged that generic benefit lists are insufficient. Below is a structured view with real benchmarks:
Benefit AreaWhat It MeansReal-World MetricCost ReductionAutomating administrative tasks (scheduling, billing, coding) and optimizing infrastructure15–30% reduction in IT operational costs; up to 40% reduction in administrative overheadWorkflow OptimizationAI-assisted triage, digital care pathways, and automated alerts reduce manual bottlenecksDeployment time reduced from days to hours (CI/CD implementation cases)Patient OutcomesEarlier diagnosis, personalized treatment plans, and reduced preventable readmissions38% reduction in hospital readmissions with remote monitoring programsInteroperabilityUnified patient data accessible across departments and care settingsReduced duplicate testing, faster diagnosis cyclesRevenue CycleAutomated claims processing, error reduction, and faster reimbursementDenial rates drop significantly with AI-powered coding assistanceSecurity & ComplianceContinuous monitoring, encryption, and automated compliance controlsProactive detection of incidents before they escalate to breachesMeasurable Benefits of Digital Transformation in Healthcare
Key Takeaway
The ROI of digital transformation in healthcare is not just financial.
Hospitals that have successfully digitized report improved staff satisfaction, higher patient NPS scores, and significantly faster time-to-care
— outcomes that reinforce each other in a virtuous cycle.
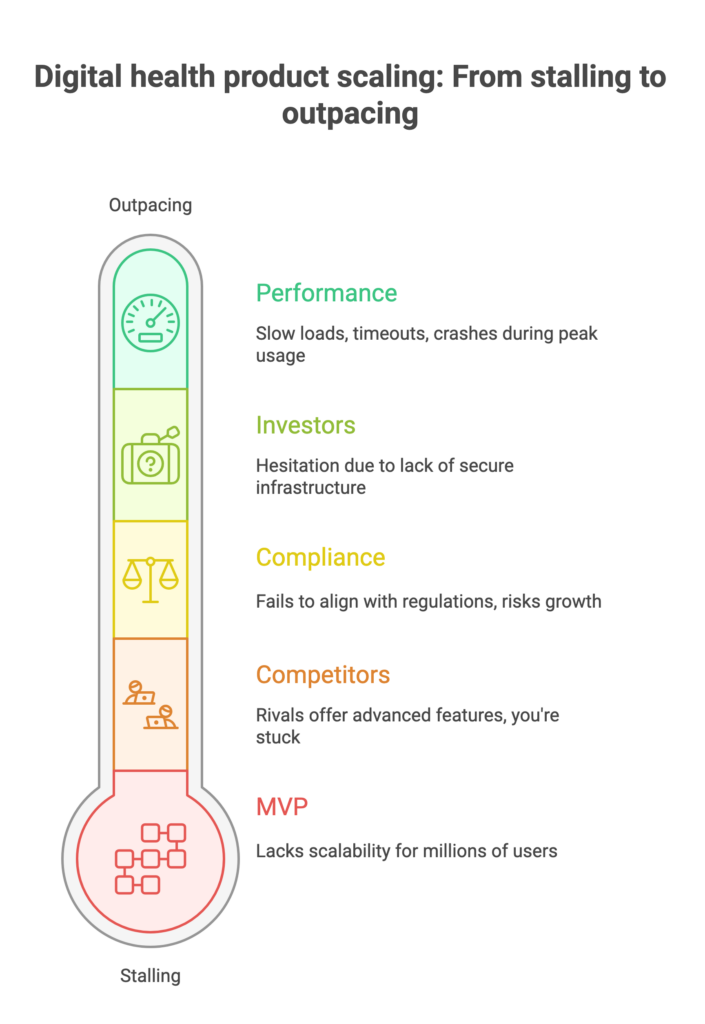
Challenges to Healthcare Digital Transformation (and How to Overcome Them)
🔒
Data Privacy & Security
Healthcare data is 10× more valuable than financial data on the dark web, making it the top target for ransomware. HIPAA, GDPR, and ISO 27799 compliance is non-negotiable.
🏗️
Legacy System Integration
Most healthcare organizations run on 10–20 year old systems. Integrating modern platforms with these via HL7 FHIR standards requires careful architecture planning.
👥
Resistance to Change
Clinical staff distrust technology that disrupts established workflows. Change management, co-design with clinicians, and phased rollout dramatically increase adoption rates.
🎓
Skills Gaps
Digital literacy varies widely across healthcare workforces. Continuous training programs and UX-first technology design are the twin levers for closing this gap.
💰
Cost of Implementation
Enterprise digital transformation has high upfront costs. Cloud-first and phased approaches reduce capital risk while delivering measurable ROI within 12–18 months.
🔄
Interoperability Gaps
Data silos between EHR, labs, and payers prevent unified views. HL7 FHIR R4 and modern API-first architecture are the industry's emerging answer.
10 Real-World Cases of Digital Transformation in Healthcare
1
Infrastructure Optimization & Data Management in Healthcare
Challenge
A health tech company operated on outdated, non-scalable infrastructure with frequent downtimes that directly impacted patient care operations and data availability.
Solution
Gart Solutions implemented a comprehensive infrastructure modernization: legacy system migration to cloud, HIPAA-compliant secure data management pipelines, and dynamic auto-scaling.
Impact
Eliminated critical downtimes, reduced data access latency, and achieved full HIPAA compliance — enabling the organization to scale operations without infrastructure risk.
Read the full case study →
2
CI/CD Pipelines for an E-Health Platform
Challenge
An e-health platform suffered from slow, error-prone manual deployments that delayed feature releases and introduced instability in a compliance-sensitive environment.
Solution
Automated CI/CD pipelines with Kubernetes orchestration, integrated compliance checks, and real-time monitoring with automated rollback capabilities.
Impact
Deployment time dropped from days to hours. Human error rates fell significantly. Feature velocity increased, enabling the platform to respond faster to clinical user needs.
View case study →
3
Electronic Medical Records (EMR) for a Government E-Health Platform
Challenge
A government E-Health initiative required a compliant, secure EMR platform with strict HIPAA and GDPR requirements, deployed on local cloud infrastructure.
Solution
Gart deployed on-premises CI/CD pipelines using GiGa Cloud hardware with VMware ESXi, Terraform, and data-masking techniques for non-production environments.
Impact
Delivered a fully compliant, secure EMR system enabling the government platform to serve thousands of patients while passing all regulatory audits.
4
Healthcare SaaS Migration: AWS to Azure with PHI Compliance
Challenge
A high-growth healthcare SaaS company needed to revamp CI/CD pipelines for .NET and Node.js environments and migrate from AWS to Azure without disrupting PHI access compliance.
Solution
Gart implemented Terraform infrastructure-as-code, rebuilt CI/CD pipelines for both stacks, and orchestrated a zero-downtime cloud migration with compliance maintained throughout.
Impact
Seamless migration with full PHI access compliance maintained. Improved infrastructure cost efficiency and development velocity post-migration.
5
HIPAA Migration: HealthCareBlocks to AWS (Ruby on Rails)
Challenge
A Ruby on Rails healthcare application needed migration from HealthCareBlocks to Amazon AWS with strict HIPAA compliance requirements and zero tolerance for data integrity risk.
Solution
Gart led a meticulous migration with continuous HIPAA compliance validation at every stage, encryption in transit and at rest, and a phased cutover to eliminate downtime risk.
Impact
Full migration completed without compliance incidents. Application performance improved on AWS infrastructure with better scalability for future growth.
6
ISO 27001 Compliance & Cloud Migration (Spiral Technology)
Challenge
Spiral Technology faced dual challenges: achieving ISO 27001 certification and migrating to cloud simultaneously, with data security as the primary constraint.
Solution
Gart provided end-to-end ISO 27001 implementation guidance, risk assessment frameworks, and a detailed cloud migration plan with advanced encryption and monitoring.
Impact
ISO 27001 certification achieved. Continuous monitoring established post-migration to maintain compliance and detect emerging threats in real time.
7
Google DeepMind Health — AI Diagnostics for Ophthalmology
Challenge
Ophthalmology screening capacity globally is constrained by specialist availability, causing diagnosis delays for conditions like diabetic retinopathy and age-related macular degeneration.
Solution
DeepMind Health developed an AI system trained on retinal scans that can detect over 50 eye conditions with accuracy matching or exceeding specialist ophthalmologists.
Impact
Deployed in major hospital systems, the AI enables rapid first-line screening, routing only complex cases to specialists — dramatically increasing diagnostic throughput.
8
Telehealth at Scale — Pandemic Response & Beyond
Challenge
The COVID-19 pandemic created overnight demand for remote consultation infrastructure that most healthcare systems were not equipped to deliver at scale.
Solution
Health systems globally rapidly deployed cloud-based telehealth platforms, integrated with EHR systems, enabling video consultations, e-prescriptions, and remote monitoring.
Impact
Telehealth usage surged over 154% vs pre-pandemic levels. Beyond the crisis, a permanent behavioral shift: patients now expect remote access as a standard offering.
9
IoT-Enabled Remote Patient Monitoring for Chronic Disease
Challenge
Patients with chronic conditions like heart failure and COPD represent a disproportionate share of hospital readmissions, driven by delayed detection of deteriorating vitals.
Solution
IoT remote monitoring programs deploy connected biosensors that transmit real-time vitals to clinical dashboards, triggering automated alerts when thresholds are crossed.
Impact
Hospital systems report up to 38% reduction in 30-day readmission rates — one of the highest-ROI interventions in value-based care.
10
Robotic Process Automation (RPA) in Healthcare Administration
Challenge
Healthcare administrative staff spend up to 34% of their time on repetitive manual tasks: prior authorizations, claims processing, and scheduling — tasks prone to error and burnout.
Solution
RPA bots handle end-to-end administrative workflows — pulling patient data, filling forms, submitting claims, and triggering exceptions for human review only when needed.
Impact
Organizations report 40–70% reduction in administrative processing time and reallocation of staff capacity to higher-value clinical support work.
How Digital Transformation Enhances Patient Experience
Telehealth and Remote Consultations
The telehealth revolution is permanent. Beyond the pandemic-era necessity, patients now actively choose virtual care for its convenience. Modern telehealth platforms enable:
Real-time video consultations with prescriptions delivered to pharmacy within minutes
Telepsychiatry for mental health access in underserved regions
Continuous remote management of diabetes, hypertension, and cardiac conditions
Second-opinion consultations with specialists regardless of geography
Personalized Medicine and AI Diagnostics
Digital transformation enables care that was genuinely impossible a decade ago. AI-assisted diagnostics analyze radiology images, ECGs, and genomic data to detect diseases at stages where intervention has the highest impact. IBM Watson Health, for example, analyzes thousands of patient records to surface treatment recommendations that clinicians may not have considered.
Predictive analytics now enable proactive rather than reactive care — identifying patients at elevated risk for sepsis, cardiac events, or 30-day readmission before deterioration begins, enabling earlier, cheaper, and more effective interventions.
Patient Data Security as a Patient Experience Issue
Patients increasingly understand that data security is not just a compliance issue — it is a trust issue. Healthcare organizations that demonstrate strong cybersecurity practices, transparent data use policies, and prompt breach response build significantly higher patient loyalty and satisfaction.
Step-by-Step Digital Transformation Roadmap for Healthcare Organizations
Phase 1
Months 1–2
Assessment & Strategy
Conduct an IT infrastructure audit to map current systems, identify compliance gaps, cost inefficiencies, and security exposures. Define transformation goals aligned to clinical and business outcomes.
Phase 2
Months 2–4
Foundation & Security
Establish cloud infrastructure with HIPAA-compliant architecture. Implement IAM, encryption, MFA, and continuous monitoring from day one. This foundation is what everything else builds on.
Phase 3
Months 4–9
Core System Modernization
Migrate priority workloads to cloud. Integrate EHR systems with modern APIs. Deploy CI/CD pipelines for healthcare applications. Begin HL7 FHIR implementation for interoperability.
Phase 4
Months 6–12
Digital Care Enablement
Roll out telehealth platforms, patient portals, and mobile access. Deploy IoT remote monitoring for chronic disease populations. Introduce AI-assisted documentation and triage tools.
Phase 5
Months 9–18
Analytics & AI
Build a unified data platform. Implement predictive analytics for readmission risk, staffing optimization, and supply chain management. Introduce AI diagnostics for clinical workflows.
Phase 6
Ongoing
Continuous Improvement & Scale
Establish KPIs and measure outcomes quarterly. Expand successful pilots across the organization. Maintain compliance posture through regular IT audits and staff training.
Lessons from Failed Healthcare Digital Transformation Projects
Analyzing transformations that underdelivered reveals consistent failure patterns that are entirely preventable:
Failure PatternWhat Goes WrongPreventionTechnology-first thinkingDeploying tools without redesigning workflows. Staff work around the technology, defeating its purpose.Start with patient/clinical outcomes. Technology serves the workflow redesign.Big Bang implementationsAttempting full-system replacement in a single cutover event creates catastrophic risk in healthcare.Phased rollout with parallel systems during transition. Pilot → expand.Security bolted on lateCompliance and security added after build creates architectural debt that is expensive and risky to remediate.Security-by-design from the first line of architecture. HIPAA compliance as a design requirement.Underestimating change managementClinical staff resistance kills adoption rates. The best system unused is worthless.Clinicians co-design the solution. Change management and training investment matches technology investment.No clear ownershipTransformation projects without a clinical champion and executive sponsor drift, stall, or get abandoned.Assign a dedicated transformation leader with cross-functional authority and clinical credibility.Lessons from Failed Healthcare Digital Transformation Projects
Regulatory Frameworks Driving Healthcare Digital Transformation
Digital transformation in healthcare does not happen in a regulatory vacuum. Compliance requirements actively shape architecture decisions, vendor selection, and deployment timelines:
FrameworkScopeImpact on Digital TransformationHIPAAUS — Protected Health Information (PHI)Mandates encryption, access controls, audit trails, and breach notification. Shapes all cloud architecture decisions.GDPREU — All personal data including health recordsRequires data minimization, consent management, and right to erasure. Affects global platforms serving EU patients.HITECH ActUS — Electronic Health RecordsIncentivizes meaningful use of EHR technology. HIPAA-compliant apps are considered HITECH compliant.ISO 27001Global — Information Security ManagementGold standard for security governance. Required by many enterprise healthcare clients as vendor qualification.HL7 FHIRGlobal — Interoperability StandardEnables data exchange between different healthcare systems. Increasingly mandated by US CMS for payers.Regulatory Frameworks Driving Healthcare Digital Transformation
Gart Solutions · Healthcare IT Services
Struggling with Your Healthcare Digital Transformation?
Gart Solutions has helped health tech companies navigate infrastructure modernization, HIPAA compliance, cloud migration, and DevOps transformation. We deliver quick wins from day one.
☁️
Cloud Migration
AWS, Azure, GCP — HIPAA-compliant by design
⚙️
DevOps & CI/CD
Automate deployments & reduce clinical downtime
🔍
IT Audit & Compliance
Infrastructure audits, HIPAA, ISO 27001 readiness
🏗️
Infrastructure Mgmt
Managed services, SRE, monitoring & reliability
👔
Fractional CTO
Strategic tech leadership for scaling companies
🔄
Transformation
End-to-end strategy & execution for IT
Get a Free Consultation →
See our healthcare work
★ 4.9 rating · 15+ verified reviews on Clutch · Trusted by health tech companies globally
Conclusion
Healthcare organizations understand that digital transformation is crucial for enhancing healthcare services and strengthening patient relationships. Beyond technology investments, this transformation necessitates a shift in organizational culture and employee engagement, requiring enterprise-wide involvement.
Leading health organizations are adopting six key strategies to advance digitally:
Establish digital leadership and governance aligned with business strategies.
Cultivate a digital culture supported by leadership at all organizational levels.
Develop next-generation talent with a focus on workforce quality and quantity.
Integrate cybersecurity at all stages for robust risk management.
Emphasize flexibility and scalability to adapt to evolving technologies.
Implement measurable, accountable KPIs to track the success of digital initiatives.
Successfully navigating digital transformation in healthcare requires expertise and a business-first approach of IT Consulting.
Gart Solutions can guide healthcare providers through the process of Digital Transformation, accelerating the adoption of digital healthcare technologies and improvement of patient outcomes.
Contact Gart today to learn more about how we can help you solve the challenges of digital transformation in healthcare.
Struggling with digital transformation for your healthcare project? Get expert guidance and IT Consultancy for your project free of charge. “Quick wins” – guaranteed. Contact Us.

Healthcare companies are under constant pressure to deliver high-quality patient care while managing vast amounts of data, complying with regulatory requirements, and adapting to new technologies.
DevOps, a set of practices that combines software development (Dev) and IT operations (Ops), offers significant advantages for healthcare organizations striving to meet these challenges. In this article, we will explore the best practices and benefits of DevOps for healthcare companies.
Regulated Industry
One of the most regulated industry due to compliance standards (HIPAA, HITECH Act, FDA, CMS, JCAHO, etc)
Compliance StandardDescriptionImpact on DevOps PracticesHIPAAHealth Insurance Portability and Accountability ActRequires strict data security and privacy measures, necessitating encryption, access controls, and audit trails. DevOps practices must ensure compliance at all stages.HITECH ActHealth Information Technology for Economic and Clinical Health ActEncourages the adoption of electronic health records and sets standards for data breach notification. DevOps practices need to secure electronic health records and establish efficient breach response procedures.FDAFood and Drug AdministrationEnforces regulations on the development and deployment of medical devices and pharmaceutical software. DevOps in healthcare must adhere to rigorous compliance checks, documentation, and validation.CMSCenters for Medicare & Medicaid ServicesRegulates healthcare payment and service delivery. DevOps practices must align with regulations to ensure efficient billing, payments, and service quality.JCAHOJoint Commission on Accreditation of Healthcare OrganizationsProvides accreditation for healthcare organizations. DevOps practices play a role in meeting accreditation standards related to patient safety, care quality, and data security.GDPRGeneral Data Protection Regulation (EU)Applies to healthcare organizations that handle EU patient data. DevOps practices must include data protection and consent mechanisms to comply with GDPR requirements.These compliance standards impact DevOps practices by requiring specific security, data protection, documentation, and quality assurance measures tailored to the respective industry's needs.
Specific DevOps Practices Tailored for the Healthcare Industry
HIPAA Compliance
Healthcare organizations deal with sensitive patient data subject to the Health Insurance Portability and Accountability Act (HIPAA). DevOps teams must prioritize HIPAA compliance by implementing encryption, access controls, and audit trails in their pipelines.
Automated Testing for Regulatory Compliance
Healthcare applications often need to adhere to strict regulatory standards. Automated testing should include compliance checks to ensure that software meets healthcare-specific regulations and standards.
Patient Data Security - Encryption & Data Masking
Protecting patient data is a top priority. DevOps should focus on securing data at rest and in transit, and implementing robust identity and access management (IAM) practices.
Utilize strong encryption algorithms to protect sensitive healthcare data when it is stored (at rest) and when it is transmitted (in transit). This ensures that even if unauthorized access occurs, the data remains unreadable and secure.Additionally, implement data masking in non-production environments to protect patient data during development and testing, aligning with stringent healthcare data security requirements.These methods allow for the realistic testing and development of applications without exposing actual patient data. Sensitive elements within the data are replaced with fictional or masked values, preserving data privacy and HIPAA compliance.
Zero Downtime
Healthcare services can't afford downtime. DevOps should aim for zero-downtime deployments, using strategies like blue-green deployments or canary releases to minimize disruptions to patient care.
Disaster Recovery and Redundancy
In the healthcare sector, maintaining high availability is paramount. To safeguard against potential system failures, DevOps must incorporate robust disaster recovery and redundancy measures. These measures are crucial for ensuring uninterrupted operations and patient care, especially in the face of unforeseen disasters or critical system issues. Gart, known for its expertise in this area, offers specialized solutions for Backup & Disaster Recovery to bolster healthcare system resilience.
Change Management and Version Control
Strict change management and version control are essential in healthcare to track modifications, updates, and configurations. DevOps tools can help manage and document these changes effectively.
Collaboration with Clinical Teams
DevOps teams should collaborate closely with clinical professionals to understand their needs and feedback. This ensures that software aligns with clinical workflows and improves patient care.
Performance Monitoring
Implement robust performance monitoring to proactively identify and resolve issues before they impact patient care. Real-time monitoring of healthcare systems is crucial for maintaining service levels.
Regulated Data Retention and Backup
Data retention and backup policies need to comply with healthcare data retention regulations. DevOps practices should include automated data backup and secure storage management.
? Looking to streamline your operations, boost security, and scale effectively? Reach out to Gart's DevOps specialists for a transformation. ? Contact Gart Today!
Cross-Functional Training
Encourage cross-functional training between IT staff and healthcare professionals to foster a deeper understanding of healthcare processes and IT requirements.
Non-Disruptive Updates
Develop strategies for non-disruptive software updates to minimize disruptions during critical patient care procedures. Implement rolling updates or feature flags to control new functionalities.
Serverless Agility
With a serverless architecture, healthcare companies are liberated from the burden of managing servers and infrastructure. Serverless platforms seamlessly adjust resource scaling according to demand, ensuring your SaaS application effortlessly adapts to varying user activity levels without the need for manual interventions. You focus on coding, while the cloud does the rest, significantly simplifying operations.
Incident Response Planning
Develop and regularly test incident response plans tailored to healthcare scenarios to ensure quick recovery in case of security breaches or system failures.
Containerization and Microservices
Utilize containerization and microservices to enhance scalability, portability, and resource efficiency, while maintaining healthcare application performance.
Secure Code Practices
Promote secure coding practices within DevOps teams to reduce vulnerabilities in healthcare software, where data security is of utmost importance.
Comprehensive Documentation
Maintain comprehensive documentation for all DevOps processes and configurations, facilitating auditing and ensuring healthcare software integrity.
By integrating these healthcare-specific DevOps practices, healthcare organizations can enhance their ability to provide high-quality patient care while complying with regulatory standards and maintaining data security. These practices ensure that the benefits of DevOps are tailored to the unique demands of the healthcare industry.
DevOps in Healthcare: Best Practices
Automation
DevOps encourages automation across the entire software development and deployment lifecycle. This includes automating code testing, deployment, and monitoring. In healthcare, where patient safety and data security are paramount, automation reduces the risk of human error and enhances compliance with regulatory requirements.
Collaboration
DevOps fosters a culture of collaboration between development and operations teams. Healthcare organizations can benefit from improved communication, leading to faster issue resolution, more efficient deployments, and better overall patient care.
Continuous Integration and Continuous Deployment (CI/CD)
The CI/CD pipeline is a fundamental DevOps practice. It allows healthcare companies to make rapid and frequent software releases while maintaining high quality. This agility is crucial for adapting to changing healthcare needs.
Security
The healthcare industry is a prime target for cyberattacks due to the sensitive nature of patient data. DevOps integrates security from the beginning of the development process, making it easier to identify and mitigate vulnerabilities. Regular security testing and automated compliance checks enhance data protection.
Monitoring and Feedback
Continuous monitoring and feedback loops in DevOps help healthcare organizations identify and address issues promptly. Real-time insights into system performance and user experience enable proactive problem-solving and ensure the highest level of patient care.
Benefits of DevOps in Healthcare
Improved Patient Care: DevOps practices enhance the quality and reliability of healthcare software, contributing to improved patient care. Faster deployments and quicker issue resolution mean healthcare professionals can access critical tools without disruption.
Cost Efficiency: Automation reduces manual intervention, resulting in cost savings. With healthcare costs continually under scrutiny, DevOps helps companies allocate resources more efficiently.
Regulatory Compliance: DevOps streamlines compliance efforts by automating documentation and ensuring security and privacy requirements are met. This minimizes the risk of penalties associated with non-compliance.
Faster Innovation: The ability to release new features and updates quickly enables healthcare companies to innovate in response to changing patient needs, market demands, and technological advancements.
Data Security: DevOps best practices for security ensure that patient data remains confidential and protected. Timely detection and remediation of vulnerabilities help prevent data breaches.
Enhanced Productivity: By automating time-consuming tasks and promoting collaboration, DevOps frees up resources and allows healthcare professionals to focus on patient care rather than IT issues.
Case Studies: E-Health DevOps Transformation
CI/CD Pipelines and Infrastructure for E-Health Platform
Explore how Gart Solutions transformed a healthcare development company's Electronic Medical Records Software (EMRS) for a government E-Health platform and CRM systems. Gart implemented CI/CD pipelines and on-premises infrastructure, adhering to strict HIPAA and GDPR standards.By leveraging local cloud provider GiGa Cloud's hardware, utilizing VMWare ESXi and Terraform, and implementing data-masking techniques, they ensured secure and compliant data management.
Seamless Rails Application Migration: Transitioning from HealthCareBlocks to AWS with HIPAA Compliance
Gart orchestrated a smooth and comprehensive migration of a Ruby on Rails application from HealthCareBlocks to Amazon AWS. With meticulous attention to detail, Gart prioritized HIPAA compliance, safeguarded data integrity, and ensured the continued seamless operation of the application in its new cloud environment.
Healthcare SaaS: Cloud Engineer's Journey in CI/CD, Terraform, and Cloud Migration
Gart took on the challenge at a high-growth healthcare SaaS company, where the task was to revamp CI/CD pipelines for both .NET and Node.js environments and implement Terraform infrastructure. Alongside these tasks, Gart orchestrated a smooth AWS to Azure migration. Gart's impeccable work ensured PHI access compliance. Gart seamlessly interfaced with a US-based team.
? Are you seeking to streamline your operations, enhance security, and improve scalability? Transform operations and security with Gart's DevOps experts. ? Contact Gart Today!
Conclusion
DevOps has rapidly become a key driver of efficiency, security, and innovation in the healthcare industry. By adopting DevOps best practices, healthcare companies can provide better patient care, reduce costs, meet regulatory requirements, and stay competitive in a rapidly evolving field. As the industry continues to evolve, embracing DevOps will be essential for healthcare organizations to thrive in an increasingly digital and data-driven world.

AI and machine learning are revolutionizing healthcare, especially in the realm of medical devices, bringing in new ways to diagnose and treat patients. But with this fast-paced innovation comes the tricky task of regulating technology that’s constantly evolving.
Agencies like the FDA in the U.S. and regulatory bodies in Europe are working to keep up, finding ways to make sure these high-tech tools are safe, reliable, and effective. By creating flexible guidelines, building collaborative partnerships, and focusing on real-world monitoring, regulators are adapting to the unique challenges of AI-driven healthcare — aiming to support innovation while keeping patient safety front and center.
Differences in Regulatory Approaches to AI in Healthcare: US vs. Europe
1. Regulatory Structure and Oversight
United States: In the U.S., the Food and Drug Administration (FDA) is the main body overseeing AI in medical devices. It operates under a centralized system with clear processes for classifying devices, assessing risks, and approving them. The FDA’s Digital Health Center of Excellence focuses on AI and machine learning (ML) in healthcare, offering resources and guidance for developers. The FDA itself reviews medical AI devices to make sure they’re safe and effective.
Europe: The European Union (EU) and the United Kingdom (UK) follow a more decentralized system, using third-party certifying bodies for conformity assessments instead of direct government oversight. The EU’s regulatory framework is developed by the European Commission, aiming to create consistent regulations across member states for a smooth internal market. In the UK, the Medicines and Healthcare products Regulatory Agency (MHRA) works with the Department of Health to oversee AI in healthcare.
"Unlike in America, we don’t really have a single agency overseeing medical devices development in Europe... The European Commission drives the policy, aiming for harmonization across member states to support a single market."
Lincoln Tsang, a UK-based legal expert
2. Risk-Based Frameworks for Classification
US FDA: The FDA categorizes AI-based medical devices by their risk level and intended use, with a focus on potential patient impact. Lower-risk devices, like general wellness apps, face minimal oversight, while higher-risk tools, particularly those that influence clinical decisions, go through strict evaluation. The FDA’s guidance highlights functionality, deployment context, and patient safety as key factors in deciding the risk level and regulatory needs.
European and UK Standards: Similar to the FDA, regulators in Europe and the UK classify devices based on functionality, intended use, and patient impact. Both the EU and UK use a risk-based approach to assess whether AI software qualifies as a medical device, examining the potential harm and healthcare role of the device. Unlike the FDA’s centralized model, the EU uses third-party bodies for assessments, adding industry involvement to the review process.
3. Approval Pathways and Compliance Assistance
The FDA offers several resources to help developers, including guidance documents, informal consultations, and a Digital Health Policy Navigator to clarify regulatory requirements. A key tool is the Predetermined Change Control Plan (PCCP), which lets developers update AI models without resubmitting for approval, as long as updates follow pre-approved guidelines.
The EU and UK support emerging tech through policy papers and adaptable guidelines. While EU regulators are considering adaptive AI-specific regulation, they currently use general guidance rather than structured pathways like the FDA’s PCCP. Both regions prioritize flexibility, updating guidelines and consulting with industry to keep up with rapid tech advancements in AI and digital health.
"We understand the impact this has on companies, particularly for smaller companies and startups, which we see a lot of in the digital health space. Predictability in regulation is crucial."
Sonja Fulmer, Deputy Director, Digital Health Center of Excellence
4. International Harmonization Efforts
Recognizing the global reach of AI, the FDA, Health Canada, and the UK’s MHRA collaborate to align standards and practices. This teamwork simplifies the approval process for companies across borders. Through groups like the International Medical Device Regulators Forum (IMDRF), these agencies work on creating standards that support global interoperability, safety, and clarity. The IMDRF also offers guidance on issues like machine learning practices, promoting a unified regulatory approach worldwide.
Third-Party Compliance Audits for Healthcare Startups
Third-party compliance audits are key for healthcare startups to ensure their products meet regulatory standards before hitting the market. Companies like Gart Solutions offer specialized compliance audits and consulting services to help startups align with the rules set by bodies like the FDA in the U.S. and certification organizations in the EU.
These third-party services support startups by helping them:
Assess Regulatory ReadinessThrough preliminary audits and gap assessments, firms like Gart Solutions help startups identify their current compliance status and highlight areas needing improvement.
Prepare for Formal CertificationBy simulating official audit conditions, third-party firms enable startups to address potential issues in advance of formal evaluations by agencies like the FDA or European certifying bodies.
Monitor Ongoing ComplianceSince regulations, particularly around adaptive AI, are constantly evolving, third-party auditors often conduct periodic reviews to ensure products stay compliant. For AI-enabled devices, these audits can also include checks on algorithmic fairness, data quality, and post-market performance.
Benefits of Compliance Audits for Startups
Partnering with third-party compliance firms offers several advantages:
Cost Savings: Catching compliance issues early can prevent expensive delays and rework during regulatory approval.
Streamlined Approvals: A thorough pre-audit can smooth the formal certification process, reducing friction with regulatory bodies.
Increased Trust and Transparency: Third-party audits show a startup’s dedication to safety and transparency, boosting stakeholder and consumer confidence.
In regions like the EU, where third-party assessments are a regulatory standard, companies like Gart Solutions help fill the gap for startups that may not have in-house compliance expertise. This support is especially valuable for AI-driven healthcare startups, where standards are both strict and rapidly changing.
Get a sample of IT Audit
Sign up now
Get on email
Loading...
Thank you!
You have successfully joined our subscriber list.
Why Postmarket Surveillance Matters
Postmarket surveillance plays a vital role in regulating AI in medical devices. For high-stakes uses like sepsis detection tools, the FDA requires a monitoring plan to track real-world performance, ensuring devices remain safe and effective across diverse patient populations. This process means manufacturers need to keep an eye on model bias, data quality, and overall device performance in everyday clinical settings. By actively managing these factors, postmarket surveillance helps reduce risks from data issues or model bias, supporting consistent, reliable performance over time.
Trends and the Future of Regulation
With AI becoming a bigger part of healthcare, regulators are likely to move toward more flexible, adaptive policies. Emerging challenges, like continuous-learning AI algorithms, are pushing agencies to rethink how they manage the entire lifecycle of these technologies. Quality assurance, postmarket surveillance, and adaptable regulations are all set to play a larger role as AI advances.
The FDA is working on guidelines for adaptive AI, expected to be released soon, which will help developers as they build continuously learning algorithms. Meanwhile, regulatory bodies in the UK and EU are exploring similar frameworks suited to their own standards, promoting international alignment and consistency.
Conclusion
The regulatory landscape for AI in healthcare is advancing rapidly to keep pace with technological developments. With their risk-based frameworks, both the FDA and European regulators are focused on ensuring the safety and efficacy of AI-enabled medical devices while supporting innovation. Through resources like the Digital Health Center of Excellence and international harmonization initiatives, agencies are setting the stage for a future where AI can safely and effectively transform healthcare, with robust postmarket surveillance and flexible change management strategies forming the backbone of this evolving regulatory framework.